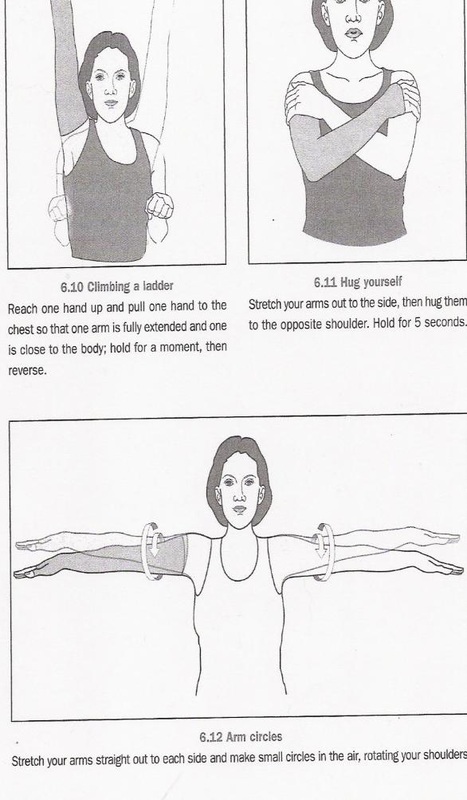
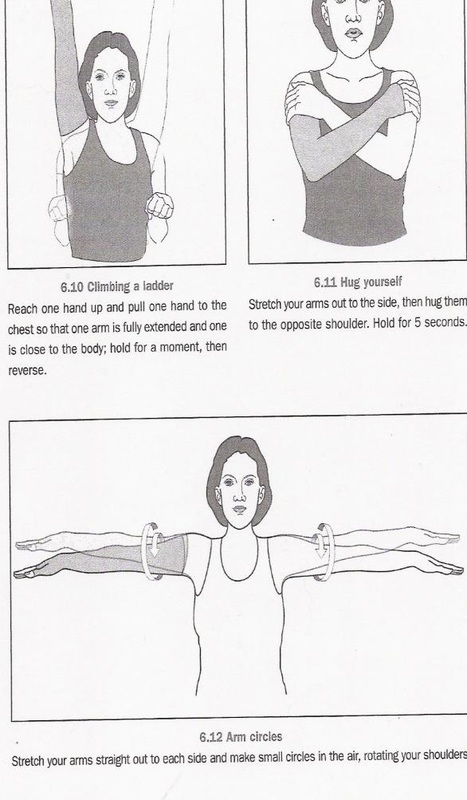
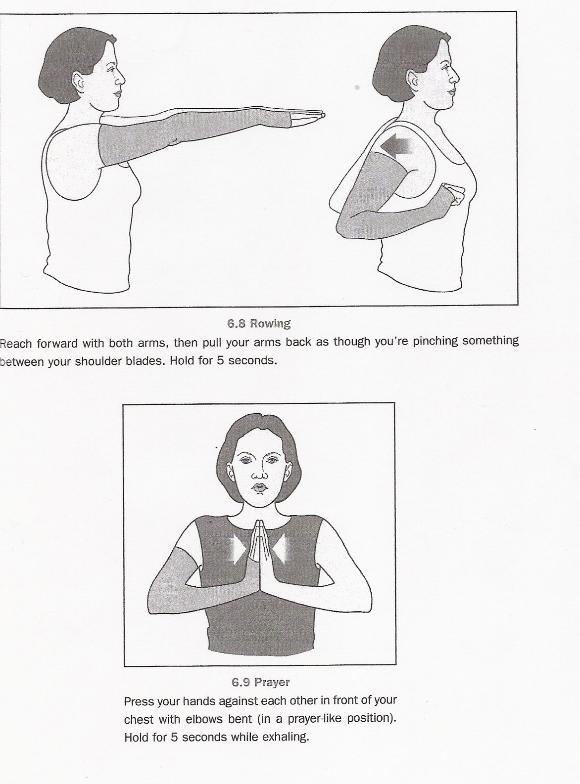
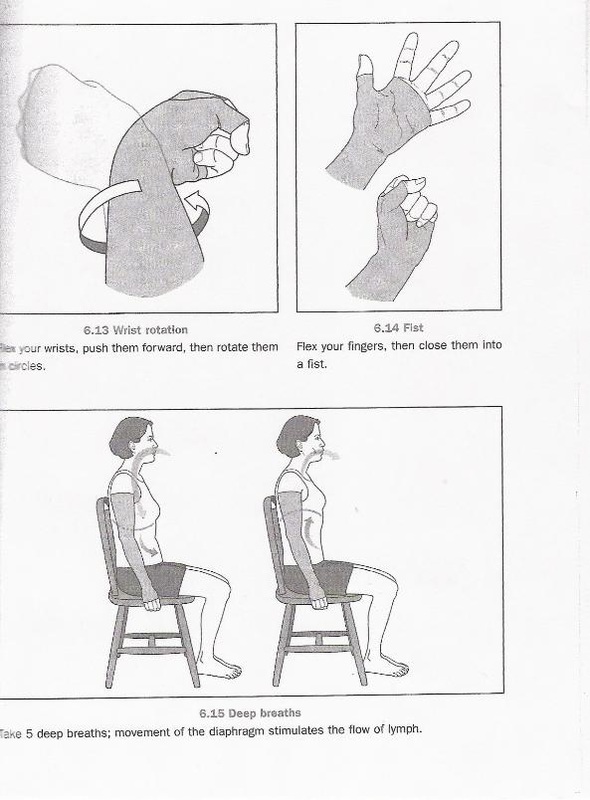
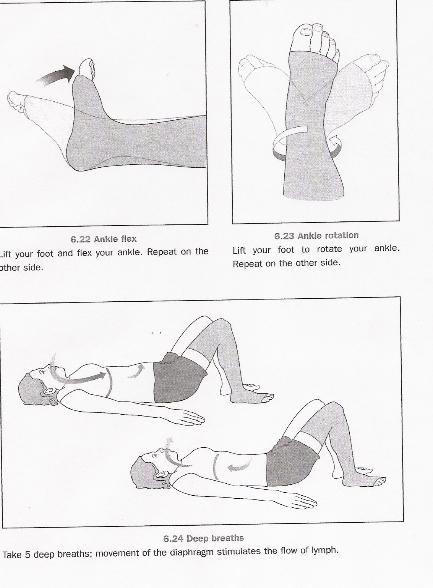
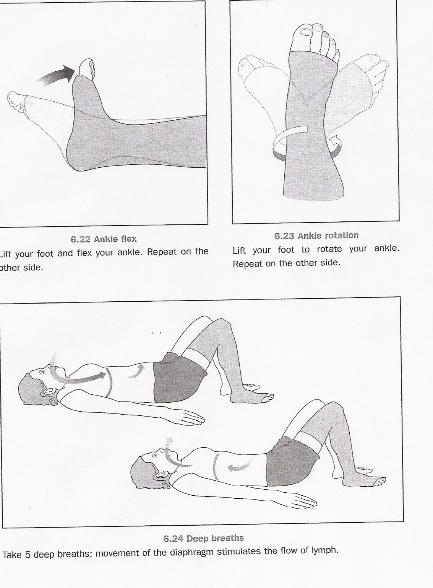
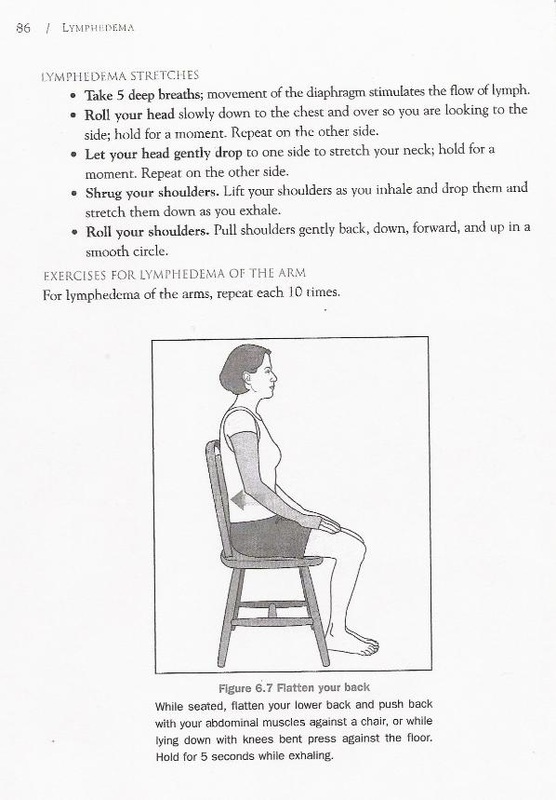
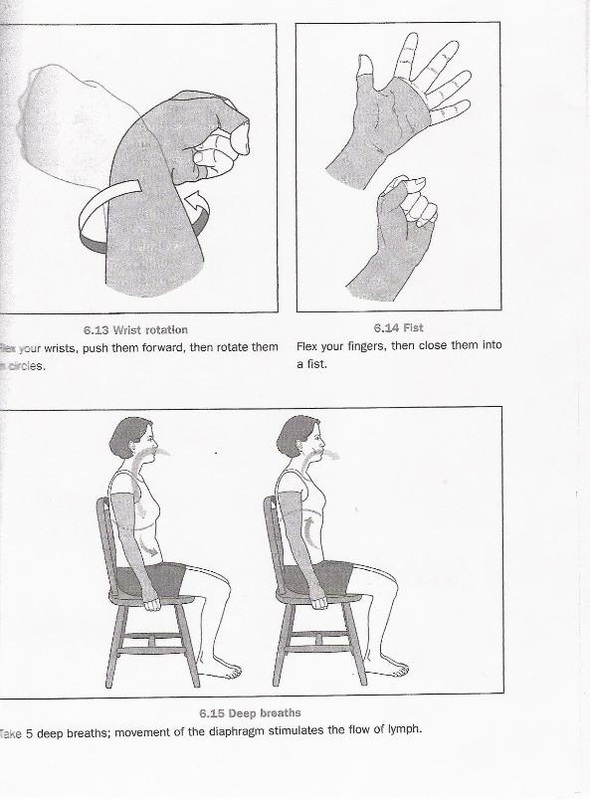
Source: "All illustrations were
reproduced by permission from Lymphedema:
Understanding and
Managing Lymphedema After Cancer Treatment Copyright 2006 by
the
American Cancer Society, Inc., http://www.cancer.org/bookstores. All rights
reserved."
ARTICLES ON EXERCISE
Exercise and
Lymphedema,water exercise,exercise and the limb at risk
Exercise and
Lymphedema
Introduction
The movement of muscles and skin during exercise
helps drain lymph out of the affected
area and eventually back into
the bloodstream. In fact, it has been estimated that,
“During
exercise the rate of lymph flow increases 15 times.” [1]
For this reason, an
exercise program is an important component in the treatment and
management of lymphedema. Exercise is also part of a healthy lifestyle
that increases
your energy level and feeling of
well-being.
Until 2005, the National Lymphedema Network (NLN) recommended
that those with, or
at risk of developing, lymphedema limit more
strenuous activities such as lifting anything
heavier than 5 pounds
or taking part in most strenuous sports. However in the face of
increasing evidence to the contrary, the recommendations have now been
greatly
modified and research is being conducted to determine just
which sport activities these
individuals may safely participate
in.
The news is good; however, there are precautions. Tissues affected by
lymphedema do
not always react to excessive stress immediately.
Instead, the reaction may be delayed.
For this reason, going back
to a favorite sport should be undertaken with caution and,
ideally,
with guidance from a qualified trainer.
Another precaution is the need to
wear a compression garment. This provides extra
support to help
muscles function more effectively. It also prevents added fluid from
pooling
in the affected limb.
Examples of Activities
Aerobic exercises. Also
known as endurance exercises, increase your heart rate and
breathing for an extended period of time. These activities are an
important part of any
exercise regimen because they:
Improve the
circulation of both blood and lymph
Aid in the flow of fluid away from
affected areas
Combat fatigue
Increase your sense of well-being
Bench
Pressing. Kathryn Schmitz, PhD, MPH is conducting a study at the Abramson
Cancer Center of the University of Pennsylvania to determine the
effects of bench press
on those with lymphedema. To read a story
about this, go to Bench Pressing.
Dancing. Dance exercise programs encourage
healthy movements while having fun.
Exercising together as a dance
group, such as the Focus on Healing through Movement
and Dance (The
Ledbed Method), provides the added motivation and pleasure of being
part of a group.
Dragon Boats. Groups of women with lymphedema have
joined together, and trained
together as teams to complete in
dragon boat racing. To read a story about this, go to
Dragon
Boats.
Exercise classes. Some lymphedema treatment facilities provide
exercise classes as part
of their treatment program. Traditionally
those have been mild to moderate exercises
with movement, stretch
bands, activities with exercise balls, and trampolines. A newer
trend in some facilities is the inclusion of a bench pressing room. Before undertaking this
kind of activity, it is essential that you
are properly supervised and know how to use the
equipment properly
and appropriately to match your condition.
Golf. Linda T. Miller, a
Philadelphia-based physical therapist specializing in the
treatment
of lymphedema after breast cancer actively encourages her patients to return
to playing golf. Their enthusiasm has been contagious and she often
joins them in
playing. To learn more about her treatment
philosophy, visit the Breast Cancer Physical
Therapy
Center.
Race for the Cure®. Many breast cancer patients participate in the
annual Kormen
Race for a Cure.® Since their lymphedema affects the
arm it would seem that running is
not a problem; however it is
important to remember that when running the arms are
active too.
Therefore appropriate training is important.
Strength training exercises.
Also known as resistance-training, require the muscles to
exert a
force against some form of resistance. This type of exercise is beneficial for
those with lymphedema because:
The contraction of the muscles
causes a pumping action that helps to move lymphatic
fluid away
from the affected area and back toward the chest.
Strength training
encourages deep breathing to ensure an adequate supply of oxygen to
the tissues. This exercises the chest and abdomen in a manner that
stimulates lymphatic
drainage.
Stretching exercises. These are
activities such as yoga that move the skin, muscle, and
other tissues in the affected area and help to relieve the feeling of tightness that often
accompanies lymphedema. They also help regain a range of
motion in an affected area,
increase flexibility, and increase
freedom of movement. Stretching exercises are also
relaxing;
however because they do not improve endurance or strength, these activities
need to be part of a balanced exercising program.
Tennis. If you were
an avid tennis player before developing, or becoming at risk of
developing lymphedema, you will want to go back to this sport. Again
training and a
gradual return, is important. If you were accustomed
to playing singles, you might start
back by playing
doubles.
Triathlons. Those with, or at risk of lymphedema, are not letting
this stop them from
taking part in triathlons in which they bike,
swim, and run. Again, adequate and
appropriate training are
important.
Walking is an ideal exercise that does not require major
equipment, except appropriate
shoes, and can be done almost
anywhere. To learn more, read the article Walking
Toward Better
Health.
Water exercises are another ideal exercise because the water
provides total body
compression and it cushions tender joints and
make movement easier. To learn more,
read the article Water
Exercises for Lymphedema.
Basic Exercise Precautions
The following is
general information about types of helpful exercises; however the key to
success is up to you – and that is to faithfully follow through on your
exercise program!
Before beginning any exercise program, check with your
therapist or physician.
Exercise moderately and avoid overuse of your
affected limb. Gradually buildup your
strength and
ability.
Carefully follow the “warm up” and “cool down” steps of your
exercise program.
Wear your compression garment during exercise. If you have
questions about this,
check with your therapist.
Try not to get
overheated and be sure to drink plenty of water to keep your body
hydrated.
Stop exercising if you encounter any sign of trouble such
as increased swelling or pain.
Check with your therapist or
physician before restarting your exercise program.
Water Exercises for
Lymphedema
Introduction
Water exercise, also known as hydrotherapy or
aquatic therapy, consists of activities
and exercises that are
performed while immersed in water. These activities, including
swimming and movements in the water, are particularly beneficial for
those with
lymphedema because:
The support of the water makes
possible motions that could not be achieved in other
settings.
The ease of movement through the water relaxes the
muscles, decreases pain
sensations, and increases the sense of
well-being.
The buoyancy and support of the water allows exercise without
heavy jarring or impact
on the joints.
The movement of the water
against the body assists the movement of the lymph and
blood as
gentle movements in the water stimulate muscle and skin movement without
stressing other body parts.
The hydrostatic pressure of the water
provides resistance during movements that
strengthens muscles and
improves cardiac and respiratory conditioning.
Wearing Compression
Garments During Water Activities
The hydrostatic pressure of the water
replaces the need for a compression garment as
long as the affected
limb is under the water most of the time.
Some therapists do recommend
wearing a compression sleeve if the affected arm is out
of the
water during most of the exercise session.
If a sleeve is necessary, wear an
old one is recommended because chlorine in the water
is destructive
to the compression value of the garment.
Water Temperatures for Pool
Activities
Strenuous exercises, such as swimming laps, should be performed
in much cooler water,
usually between 68° F (20° C) and 86° F (30°
C) degrees. The cooler the water the longer
you can stay
in.
Gentle exercises are usually done in water that is 94° F (34° C) degrees
or slightly less.
Water at, or just below this temperature, feels
comfortably warm, helps to soften fibrotic
tissues and relaxes the
muscles. A therapeutic session is usually 50-55 minutes spent in
the water.
Hot water that exceeds 94° F (34.4° C) degrees should be
avoided because heat makes
lymphedema worse. Also very warm water,
which raises the core temperature of the
body, can cause other
complications such as added strain on the heart during strenuous
activity.
Important Precautions
Stay hydrated. Your body looses
water while you are exercising in the pool. To ensure
that you do
not become dehydrated, keep a plastic water bottle handy at pool side so you
can take a refreshing sip as needed.
Protect your affected limb.
You do not want the skin on the affected limb to get dried out
from
being in the water too long. Applying a protective lotion over that area before
going
into the water is a good idea. If you are out in the sun, a
combination of moisturizing
lotion and sunscreen should work
well.
Pool Hygiene. To avoid fungal infections, such as athlete’s foot,
always wear protective
footwear when walking to and from the pool
and in the shower area. After your water
session, when the skin is
dry, use an antifungal powder particularly between the toes and
in
deep creases.
Pool Activities: Walking in the Water
Walking in the water
is a good warmup activity to start your pool session. The more
relaxed you are, and the more slowly you walk, the better it is for
your lymphatic system.
The recommended time for this activity ranges from 3
to 10 minutes of gentle walking.
As you walk in chest level water,
concentrate on your abdominal breathing and walk
using these basic
steps:
Place your heel on the pool floor and roll on the outer edge of the
sole of your foot
toward the ball of the foot.
Then lift your
heel and for a moment stand on the tips of your toes. Next lift your foot,
bring it forward, and place it on the pool floor again.
Place the heel of the other foot on the pool floor, roll the outer edge of the sole towards
the ball of the foot, and lift the heel. Use your toes to
push off, take a step forward, and
land on the heel.
This basic
step can be alternated with walking backward or sideways. Walking backward
improves the stability of the spine and strengthens the back muscles.
Walking sideways
improves the stability of the pelvis and
hips.
Pool Activities: Arm Movements
These arm movements can be varied as
you continue to enjoy walking.
As you walk, let your arms trail behind you
and enjoy the sensation of the water moving
over them.
If your
arm is affected, let your arms float in front of you and gently move them from
side-to-side as you walk.
After your initial warm-up period you
may want to increase your pace and swing your
arms as if you were
power walking.
For power walking, bend your elbows then swing your arms back
and forth as you walk.
As you swing your arms forward bring them up
toward the surface of the water.
Pool Activities: Relaxing Shoulder Rolls in
the Water
Stand with the water up to the shoulders and relax.
Let your
arms float on the water in front of you.
Roll your shoulders upward,
backward, downward, and forward.
Your extended, but relaxed, arms will
passively follow this movement.
Repeat these movements in reverse
rotation.
Pool Activities: Head Movements in the Water
Stand with the
water up to the shoulders and relax.
Head Tilt. Slowly tilt your head from
the center to one side. Then tilt it to the other side
and return
your head to the center.
Head Turn. Turn your head to one side and then to
the center, then to the other side and
back to the center
again.
Shoulder Roll and Head Turn. These head movements may be done with
the shoulder
rolls mentioned above while relaxing.
Pool
Activities: Hand Pressing in the Water
Press the palms of your hands
together on the surface of the water and release.
Repeat this movement
several times to increase lymph drainage from the arms and
shoulders.
Pool Activities: Arm Loops in the Water
Stand with the
water up to the shoulders, relax, and let your arms float.
Turn the elbow of
the affected arm down and then bring it up and towards the front
midline of the chest.
Continue the loop outwards and take the
elbow around the side toward the midline of the
back of the
chest.
The second loop is continued until the elbow and arm are back to the
starting position.
Pool Activities: Knee Bouncing in the Water
These
movements are good exercise for flexibility and muscle movement. They also
stimulate the inguinal lymph nodes.
Stand straight and use the side
of the pool to support your back.
Bounce one knee towards your
chest.
Return that foot to the floor and then bounce the other
knee.
Noodle and Ball Activities
A noodle, also known as a pool
floater, or a ball are excellent exercise aids in the water.
Pushing a
noodle down. Hold the noodle, or ball, in front of you and push it down until
your arms are fully extended. Then, while still holding the noodle,
slowly let your arms
come up to the surface.
Sitting on a
noodle. Sit on a noodle as if you are sitting on a swing. Bring both knees
upward toward the chest and then push them outward again. This improves
abdominal
breathing, supports drainage of the groin nodes, and helps
to improve your balance.
Standing on a noodle. Begin in a sitting position
on the noodle and then bring your feet
up and move into a squatting
position on the noodle.
Push the noodle down to the pool floor and stand on
it. Just in case you loose your
balance, it is best not to do this
too close to the edge of the pool. This activity improves
your
balance and flexibility. It also improves abdominal breathing, supports
drainage of
the lymph nodes in the groin, and helps to improve
flexibility.
Walking on the noodle. Once standing on the noodle, take small
steps from one side to
the other side of the floater. To maintain
your balance, you need to turn your feet as you
move. This activity
improves balance, muscle strength, and flexibility.
Swimming
Strokes
Swimming improves your muscle tone and encourages deep
breathing.
The breaststroke is recommended because it involves gentle
stretching motions.
The butterfly stroke is not recommended when one or both
arms are affected, because it
requires strenuous repetitive
movements of the arm.
Beyond these recommendations, the strokes you use
depend on your swimming skills.
Salt Water Activities
Sea water is an
excellent medium for aquatic therapy because the salt in the water
increases the buoyancy of the body. The salt water also kills many
bacteria on the skin.
A salt water pool is a beneficial setting for aquatic
exercises and therapy sessions.
Enjoying sea water in its natural
setting, such as on the beach, is also a wonderful way to
relax,
have fun, and to get some exercise.
Caution: If lymphedema affects your
lower extremities, always wear protective footwear
when walking on
the beach or exercising in the sea water.
Caution: When exercising out of
doors, always wear a good sunscreen and reapply it as
necessary!
Caution: Before going into the ocean or a non-chlorinated
swimming facility, review the
warning about the risk of developing a
Mycobacterium marinum infection. This risk is
discussed in the
article Pet Care and Lymphedema.
http://www.lymphnotes.com/article.php/id/24/
http://www.lymphedema-therapy.com/Exercise.htm
-----------------------------------------------------
Exercise, Lymphedema, and
the Limb at
Risk
---------------------------------------------------------------------------------
Source:
Bonnie B. Lasinski, MA, PT,
CLT-LANA
---------------------------------------------------------------------------------
How
many clinicians are at a loss for words when they are asked about what kind of
exercise is "good" for individuals with lymphedema? How many
individuals living with
lymphedema or a limb at risk for lymphedema
have asked their healthcare professional
for advice concerning
exercise only to receive conflicting information? It is difficult to
"recruit"
presenters to provide workshops/discussions on exercise for both patients and
professionals alike. Exercise and lymphedema - it is a controversial
subject.
Twenty-four years ago, I was asked to do a presentation on exercise
after mastectomy
for a one day seminar sponsored by the American
Cancer Society's Long Island
Division, entitled "Living With
Cancer". When I contacted the coordinator of the
workshop, Diana
Rulon, she informed me that she was not "interested in exercise after
mastectomy
- she was interested in exercise for lymphedema!"
You can imagine my
shock and fear at that moment. I had no special training in
lymphedema management, in fact, no one did. We were just beginning to
hear strange
tales of a treatment from Europe that seemed
ridiculously mild for the severe swellings I
had seen in my limited
experience. But, I figured no problem. I'll just go to the medical
library, research the articles, and develop my talk from there. Well,
that was 1980 and
there were no articles, except for a few
abstracts of German and French studies. Now, I
was really in
trouble. Well, long story short, I was inspired by the dedication of Diana
Rulon who tried to find help for other women like herself, who had long
been ignored by
their doctors and told to live with their problem.
Thus began my journey in lymphedema
management. Trial by fire, you
might say! We presented a very basic, common sense
talk on
lymphedema, trying to define it in simple terms (no small feat when the
literature
was so poor - the definition at that time was a 2
centimeter difference between forearms
- as if that was the only
place one could have lymphedema!). Next, Diana presented
some
practical suggestions for nutrition that she had found helpful to her and
several
other women she knew. Finally, I wrapped up the session
with some very basic
information on exercise progression and then
opened the floor for questions. The
response was overwhelming. The
participants were so grateful that their problem was
finally
acknowledged, even on such a basic level.
Twenty-four years later, although
the medical management of lymphedema has come a
long way, thanks in
great part by the advocacy of Saskia Thiadens and the NLN, there is
still much work to do. Basic and advanced research on the effects of
exercise as a
lymphedema risk reduction modality must be explored.
The basic criticism of the
precautions about exercise contained in
the 18 Steps to Prevention of Lymphedema and
other risk reduction
guidelines is that they are "anecdotal" at the present time, due to
the lack of controlled double-blind studies to prove their efficacy.
Some medical
professionals have taken the position that the
individual with a limb at risk (or with
lymphedema) should go ahead
and pursue whatever exercise/activity they wish and "see
what
happens". Unfortunately, lymphedema is a chronic condition, which, presently,
has
no cure. While it is true that not all individuals who have had
lymph node disruption
(surgical or radiological) will develop
lymphedema, until physicians can better predict
who is at greater
risk for lymphedema, a prudent approach to exercise is advisable. In
the
case of individuals with primary lymphedema or established secondary
lymphedema,
working up to a level of exercise that promotes fitness
while avoiding exacerbating the
lymphedema is a good goal.
I'm
sure that some of you may have been told in the past that you should not
exercise if
you have lymphedema, or that certain types of exercise
are contraindicated if you have
lymphedema. This is not the case. I
would like to review some basic principles of
anatomy and
physiology and pathophysiology of lymphedema and how these relate to
exercise
and lymphedema. Lymphedema occurs when there is an imbalance between
lymph
transport capacity and lymph load. After any surgical disruption or radiation
treatment to a lymph node region, a state of latent lymphedema
occurs. That is to say
that the lymph transport capacity is reduced
but it is still greater or equal to the lymph
load. Acute/chronic
lymphedema develops when that balance is shifted and lymph load
exceeds the impaired lymph transport capacity. In the case of Primary
Lymphedema,
where there is a malformation/malfunctioning of the
lymphatic transport system that
results in a reduced lymphatic
transport capacity, lymph load often exceeds that
transport
capacity, and progressive lymphedema develops over time.
Our lymphatic
system, in addition to filtering out waste products, helps our bodies
maintain
fluid balance so that we are neither dehydrated nor edematous. 90% of the
water component of our blood that perfuses the capillary network and
nourishes our cells
returns to the heart via the venous system. The
10% that is left behind in the tissues
along with the extracellular
protein that filters out of the capillaries, can only return to
the
heart via the lymphatics. That 10% can amount to up to 2 liters a day. While 2
liters
may not seem like much, it adds up day after day, if there
is impairment in lymph
drainage. In addition, the extracellular
proteins can only return to the central circulation
via the
lymphatic vessels. The diameter of these molecules is too large to fit into the
openings in the vein walls - the openings in the lymphatic vessel
walls are large enough
for these protein molecules to enter
easily.
So lymphedema is not only a problem of excess water remaining in the
tissues, but of
excess protein that remains in the tissues as well.
Unfortunately, the body always moves
for a state of balance so it
actually tends to pour more water into the tissues to "dilute"
this
protein concentration - thus a vicious cycle develops. This problem is
compounded
by the fact that the white blood cells called
macrophages, which are part of our immune
response, do not work
properly in the lymphedematous fluid. This is why anyone with
lymphedema is at increased risk for infection in his or her affected
limb.
What does all this have to do with exercise? A review of the acute and
chronic effects of
exercise is helpful to understand how the limb at
risk or a lymphedematous limb might
respond to various types of
exercise. The acute responses to exercise include increases
in
heart rate, stroke volume, cardiac output, blood flow to active muscles,
systolic blood
pressure, arteriovenous oxygen difference,
ventilation, oxygen uptake, and a decrease
in blood pH and plasma
volume. Chronic adaptations to exercise include biochemical
changes
in skeletal muscles, decreased resting heart rate, decrease in total body fat,
blood lipids, and the density and strength of bone and connective
tissue. During exercise,
blood is redirected to the muscles. At
rest, only 21% of the cardiac output goes to the
muscles, compared
with as much as 88% during exhaustive exercise. As the body heats
up, an increasing amount of blood is directed to the skin, to conduct
heat away from the
body core.1 Remember that lymph transport has to
be equal to or greater than lymph
load. When you exercise, your
muscles need extra blood to supply the oxygen needed
for your
muscles to do the work of the exercise. Extra blood flow means that extra water
will remain in the extracellular spaces needing transport via the
lymphatic system. The
question is how much is too much? That is
very individual. It is important that any
exercise program be
gradually progressed to avoid sprain/strain. More importantly, a
slow progression allows the individual to monitor their affected limb
or limb at risk for
any sensation of aching or fullness that could
indicate an overwhelming of the lymphatic
system.
Exercise can
increase the uptake of fluid by the initial lymphatics and enhance the
pumping of the collecting lymphatics. In addition, exercise mobilizes
the joints and
strengthens the muscles of the involved
limb/limbs/trunk quadrant, thus decreasing the
risk of
strain/sprain.2
Exercise is best done with compression on the affected limb
either from compression
bandages or compression garments. The
bandages provide a new "tight" skin for the
muscles to contract
against, assisting in pumping the lymph out of the extremity into the
central
circulation. When lymphedema exists, the remaining lymph vessels that are
functioning are working double time to try to carry the load. These
vessels become over
dilated (stretched) and eventually, their walls
can overstretch and fail, causing a
worsening of the swelling.
Wearing compression bandages/garments provides support to
the skin
and to the lymphatic vessels directly under the skin, called the superficial
lymphatic network. It is these vessels that help to carry the load
when the larger vessels
have been cut away from the lymph nodes or
have been damaged due to trauma or
chronic venous disease, or in
the case of primary lymphedema, when there are too few
large lymph
collectors in a region due to improper vessel/node development during fetal
growth
Of course, certain types of exercise are considered higher
risk than others. For example,
high speed activities like tennis,
bowling and racquetball, place more stress on the upper
limb while jogging, stair-climbing machines, downhill skiing, water skiing, football, soccer
place more stress on the lower extremities or have higher
injury risk than other
activities such as swimming, brisk walking,
and cycling. That is not to say that someone
with lymphedema of the
leg should not jog for exercise, or that the person with
lymphedema
of the arm and hand should not play tennis or golf. It is also important to
know whether an individual was skilled at a sport/activity prior to
their developing
lymphedema. A sport-specific exercise program can
be developed for the individual to
build strength, flexibility and
endurance in the muscle groups most used in that
sport/activity.
Ultimately, the decision to "play" should be an individual one, but an
informed one.
Many men and women with lymhedema or a limb at risk
want to work out with weights. A
slow progression of light weights
can be done safely and can allow an individual to
develop good
strength and power in any muscle group. The important thing to consider is
whether you feel good after the exercise and how your affected limb
reacts after you
exercise. You must also consider your level of
daily activity and modify accordingly - if
you have had a
particularly difficult day and your affected limb is more swollen, you may
choose to do a different activity i.e. swim instead of walk, or you may
realize that the
best activity for that day is to rest with your
limb elevated. The importance of deep
abdominal breathing exercise
should not be overlooked. Deep breathing enhances the
pumping in
the thoracic duct (the major lymphatic vessel draining the lower body and the
left upper trunk/arm/hand).
A recent series of case reports
published in the Journal of Surgical Oncology3
challenges the
theory that vigorous upper body exercise is contraindicated for
individuals who have had axillary dissection during surgery for breast
cancer. The study
followed a group of 24 women for 9 months. These
women were recruited to participate
in a training program to
prepare for competition in the World Championship Dragon
Boat
Festival in Vancouver, British Columbia. Dragon Boat racing involves strenuous
repetitive upper body exercise. 18-20 women paddle 40-60 foot boats
for a distance of
500-650 meters. Circumferential measurements were
collected on 20 of the 24
participants (limbs were measured at 4
places) pre training, at the start of the racing, and
7 months
after the races. According to the authors, only two women, who had pre-
existing mild lymphedema, had increases in their upper arms (5/8 inch)
and none of the
other participants developed lymphedema. One of the
authors of the study, herself a
breast cancer survivor participated
in the program. The authors conclude that strenuous
upper body
exercise may not cause lymphedema or worsen a pre-existing lymphedema.
It is
important to note that the participants in this study completed a two-month
training
program of stretching, strengthening, and aerobic
exercises prior to engaging in the
actual strenuous activity of
Dragon Boat racing. Many individuals who undergo breast
surgery/axillary dissection/radiation are not enrolled in supervised
progressive exercise
programs like the participants of this study.
Providing structured, individualized exercise
programs should be a
goal of all centers that perform cancer surgeries. While I do not
discourage individuals from participating in sports and exercise, I do
caution them that
they should consider themselves "athletes" in the
"game" of life. As such, each
individual should engage in a
stretching/strengthening program to prepare them for full
participation in whatever activity they
choose.
-------
http://www.lymphedema-therapy.com/lymphedema-exercise.html
Lymphedema
and
Exercises
--------------------------------------------------------------------------------
Exercise
for Lymphedema Benefits Supported by Studies
Bonnie B. Lasinski, MA, PT,
CLT-LANA
--------------------------------------------------------------------------------
Exercise
and lymphedema - it is a controversial subject
How is lymphedema and
exercise viewed today? How many clinicians are at a loss for
words
when they are asked about what kind of exercise is "good" for individuals with
lymphedema? How many individuals living with lymphedema or a limb at
risk for
lymphedema have asked their healthcare professional for
advice concerning exercise
only to receive conflicting information?
It is difficult to "recruit" presenters to provide
workshops/discussions on lymphedema and exercises for both patients and
professionals
alike. Exercise and lymphedema - it is a
controversial subject.
Our Nearly 30 Years of Research on Exercise for
Lymphedema
Twenty-nine years ago in 1980, I was asked to do a presentation
on exercise after
mastectomy for a one day seminar sponsored by the
American Cancer Society's Long
Island Division, entitled "Living
With Cancer". When I contacted the coordinator of the
workshop,
Diana Rulon, she informed me that she was not "interested in exercise after
mastectomy - she was interested in exercise for lymphedema!"
You
can imagine my shock and fear at that moment. I had no special training in
lymphedema management, never mind lymphedema and exercise; in fact, no
one did. We
were just beginning to hear strange tales of a
treatment from Europe that seemed
ridiculously mild for the severe
swellings I had seen in my limited experience. But, I
figured “no
problem”. I'll just go to the medical library, research the articles, and
develop my talk from there. Well, that was 1980 and there were no
articles on exercise
for lymphedema, except for a few abstracts of
German and French studies. Now, I was
really in trouble. Well, long
story short, I was inspired by the dedication of Diana Rulon
who
tried to find help for other women like herself, who had long been ignored by
their
doctors and told to live with their problem. Thus began my
journey in lymphedema
management. Trial by fire, you might
say!
We presented a very basic, common sense talk on lymphedema, trying to
define it in
simple terms (no small feat when the literature was so
poor - the definition at that time
was a 2 centimeter difference
between forearms - as if that was the only place one could
have
lymphedema!). Next, Diana presented some practical suggestions for nutrition
that
she had found helpful to her and several other women she knew.
Finally, I wrapped up
the session with some very basic information
on lymphedema and exercise progression
and then opened the floor
for questions.
In 2009, although the medical management of lymphedema has
come a long way, thanks
in great part by the advocacy of Saskia
Thiadens and the NLN and many others, there is
still much work to
do. Basic and advanced research on the effects of exercise as a
lymphedema risk reduction modality must be explored.
The basic
criticism of the precautions about exercise for lymphedema contained in the
Risk Reduction Guidelines is that they are "anecdotal" at the present
time, due to the
lack of controlled double-blind studies to prove
their efficacy.
Some medical professionals have taken the position that the
individual with a limb at risk
(or with lymphedema) should go ahead
and pursue whatever exercise/activity they wish
and "see what
happens". Unfortunately, lymphedema is a chronic condition, which,
presently, has no cure.
While it is true that not all individuals
who have had lymph node disruption (surgical or
radiological) will
develop lymphedema, until physicians can better predict who is at
greater risk for lymphedema, a prudent approach to exercise for
lymphedema is
advisable. In the case of individuals with primary
lymphedema or established secondary
lymphedema, working up to a
level of exercise that promotes fitness while avoiding
exacerbating
the lymphedema is a good goal.
Exercise for Lymphedema makes Medical
Sense
I'm sure that some of you may have been told in the past that you
should not exercise if
you have lymphedema, or that certain types
of exercise are contraindicated if you have
lymphedema. This is not
the case. I would like to review some basic principles of
anatomy
and physiology and pathophysiology of lymphedema and how these relate to
exercise and lymphedema.
Basic principles behind occurrence of
lymphedema
•Lymphedema occurs when there is an imbalance between lymph
transport capacity and
lymph load.
•After any surgical disruption
or radiation treatment to a lymph node region, a state of
latent
lymphedema occurs. That is to say that the lymph transport capacity is reduced
but it is still greater or equal to the lymph
load.
•Acute/chronic lymphedema develops when that balance is shifted and
lymph load
exceeds the impaired lymph transport capacity.
•In
the case of Primary Lymphedema, where there is a malformation/malfunctioning of
the lymphatic transport system that results in a reduced lymphatic
transport capacity,
lymph load often exceeds that transport
capacity, and progressive lymphedema develops
over
time.
Lymphedema is a problem of excess water and protein
Our lymphatic
system, in addition to filtering out waste products, helps our bodies
maintain
fluid balance so that we are neither dehydrated nor edematous.
Up to 90% of
the water component of our blood that perfuses the capillary network and
nourishes our cells returns to the heart via the venous system.
The
10% (or more) that is left behind in the tissues along with the extracellular
protein
that filters out of the capillaries, can only return to the
heart via the lymphatics. That
10% (or more) can amount to up to 2
liters a day. While 2 liters may not seem like much,
it adds up day
after day, if there is impairment in lymph drainage.
In addition, the
extracellular proteins can only return to the central circulation via the
lymphatic vessels. The diameter of these molecules is too large to fit
into the openings in
the vein walls - the openings in the lymphatic
vessel walls are large enough for these
protein molecules to enter
easily.
So lymphedema is not only a problem of excess water remaining in the
tissues, but of
excess protein that remains in the tissues as well.
Unfortunately, the body always moves
for a state of balance so it
actually tends to pour more water into the tissues to "dilute"
this
protein concentration - thus a vicious cycle develops. This problem is
compounded
by the fact that the white blood cells called
macrophages, which are part of our immune
response, do not work
properly in the lymphedematous fluid. This is why anyone with
lymphedema is at increased risk for infection in his or her affected
limb.
Relation between lymphedema and exercise
What does all this have to
do with exercise? A review of the acute and chronic effects of
exercise is helpful to understand how the limb at risk or a
lymphedematous limb might
respond to various types of exercise. The
acute responses to exercise include increases
in heart rate, stroke
volume, cardiac output, blood flow to active muscles, systolic blood
pressure,
arteriovenous oxygen difference, ventilation, oxygen uptake, and a decrease
in blood pH and plasma volume.
Chronic adaptations to exercise
include biochemical changes in skeletal muscles,
decreased resting
heart rate, decrease in total body fat, blood lipids, and the density and
strength of bone and connective tissue.
During exercise, blood is
redirected to the muscles. At rest, only 21% of the cardiac
output
goes to the muscles, compared with as much as 88% during exhaustive exercise.
As the body heats up, an increasing amount of blood is directed to
the skin, to conduct
heat away from the body core.1 Remember that
lymph transport has to be equal to or
greater than lymph load. When
you exercise, your muscles need extra blood to supply
the oxygen
needed for your muscles to do the work of the exercise. Extra blood flow
means that extra water will remain in the extracellular spaces needing
transport via the
lymphatic system.
So exercise for lymphedema
may be beneficial, however the question is how much is too
much?
That is very individual. It is important that any exercise program be gradually
progressed to avoid sprain/strain. More importantly, a slow
progression allows the
individual to monitor their affected limb or
limb at risk for any sensation of aching or
fullness that could
indicate an overwhelming of the lymphatic system.
Lymphedema and Exercises
are specific to each individual
Benefits of exercise for
lymphedema
•Exercise can increase the uptake of fluid by the initial
lymphatics and enhance the
pumping of the collecting
lymphatics.
•In addition, exercise mobilizes the joints and strengthens the
muscles of the involved
limb/limbs/trunk quadrant, thus decreasing
the risk of strain/sprain.2
Exercise for lymphedema is best done with
compression
Exercise for lymphedema is best done with compression on the
affected limb either from
compression bandages or compression
garments. The bandages provide a new "tight"
skin for the muscles
to contract against, assisting in pumping the lymph out of the
extremity into the central circulation. When lymphedema exists, the
remaining lymph
vessels that are functioning are working double time
to try to carry the load. These
vessels become over dilated
(stretched) and eventually, their walls can overstretch and
fail,
causing a worsening of the swelling.
Wearing compression bandages/garments
provides support to the skin and to the
lymphatic vessels directly
under the skin, called the superficial lymphatic network. It is
these vessels that help to carry the load when the larger vessels have
been cut away
from the lymph nodes or have been damaged due to
trauma or chronic venous disease,
or in the case of primary
lymphedema, when there are too few large lymph collectors in a
region due to improper vessel/node development during fetal
growth
Certain types of exercise are considered higher risk
Of course,
certain types of exercise are considered higher risk than others for
individuals
with lymphedema. For example, high speed activities like tennis, bowling and
racquetball, place more stress on the upper limb while jogging,
stair-climbing machines,
downhill skiing, water skiing, football,
soccer place more stress on the lower extremities
or have higher
injury risk than other activities such as swimming, brisk walking, and
cycling.
That is not to say that someone with lymphedema of the leg should not jog for
exercise, or that the person with lymphedema of the arm and hand
should not play tennis
or golf.
It is also important to know
whether an individual was skilled at a sport/activity prior to
their
developing lymphedema. A sport-specific exercise program can be developed for
the individual to build strength, flexibility and endurance in the
muscle groups most used
in that sport/activity. Ultimately, the
decision to "play" should be an individual one, but
an informed
one.
Things to consider regarding lymphedema and exercise
•Many men and
women with lymphedema or a limb at risk want to work out with weights.
A
slow progression of light weights can be done safely and can allow an
individual to
develop good strength and power in any muscle
group.
•The important thing to consider is whether you feel good after the
exercise and how
your affected limb reacts after you
exercise.
•You must also consider your level of daily activity and modify
accordingly - if you have
had a particularly difficult day and your
affected limb is more swollen, you may choose to
do a different
activity i.e. swim instead of walk, or you may realize that the best activity
for that day is to rest with your limb elevated.
•The importance
of deep abdominal breathing exercise should not be overlooked. Deep
breathing enhances the pumping in the thoracic duct (the major
lymphatic vessel draining
the lower body and the left upper
trunk/arm/hand).
Exercise for lymphedema is one component of the treatment
for lymphedema. You’ll
find more information here on other
components of Comprehensive Lymphedema
Treatment with our certified
lymphedema therapists.
Lymphedema and Exercise Case Studies
Case Study of
Upper Body Exercise for Lymphedema
A series of case reports published in the
Journal of Surgical Oncology3 challenges the
theory that vigorous
upper body exercise is contraindicated for individuals who have had
axillary dissection during surgery for breast cancer. The study
followed a group of 24
women for 9 months. These women were
recruited to participate in a training program to
prepare for
competition in the World Championship Dragon Boat Festival in Vancouver,
British Columbia. Dragon Boat racing involves strenuous repetitive
upper body
exercise. 18-20 women paddle 40-60 foot boats for a
distance of 500-650 meters.
Circumferential measurements were
collected on 20 of the 24 participants (limbs were
measured at 4
places) pre training, at the start of the racing, and 7 months after the
races.
According to the authors, only two women, who had
pre-existing mild lymphedema, had
increases in their upper arms
(5/8 inch) and none of the other participants developed
lymphedema.
One of the authors of the study, herself a breast cancer survivor
participated in the program. Regarding lymphedema and exercise, the
authors conclude
that strenuous upper body exercise may not cause
lymphedema or worsen a pre-existing
lymphedema.
It is important
to note in this lymphedema and exercise study that the participants in this
study completed a two-month training program of stretching,
strengthening, and aerobic
exercises prior to engaging in the
actual strenuous activity of Dragon Boat racing.
Many individuals who
undergo breast surgery/axillary dissection/radiation are not
enrolled in supervised progressive exercise programs like the
participants of this study.
Providing structured, individualized
exercise programs should be a goal of all centers
that perform
cancer surgeries. The at risk/limbs with lymphedema should be measured
periodically to insure that there are not subtle volume changes that
may not be visible to
the individual.
While I do not discourage
individuals from participating in sports and exercise, I do
caution
them that they should consider themselves "athletes" in the "game" of life. As
such, each individual should engage in a stretching/strengthening
program to prepare
them for full participation in whatever activity
they choose.
Case Study of Weight Training Effects on Lymphedema
Ahamed
et al in 2006 examined the effects of supervised upper and lower body weight
training on the incidence and symptoms of lymphedema in 45 breast
cancer survivors
who participated in a supervised, graduated
program of exercise twice weekly for 6
months. None of the
participants experienced a worsening of their lymphedema or a
triggering of lymphedema in their at risk limbs.
Schmitz et al in
2009 assessed the safety of a graduated exercise program on 295
survivors with breast cancer related lymphedema (BCRLE) and 154 at risk
for
lymphedema. Their results were similar, demonstrating that
individuals who are at risk
for lymphedema or who have lymphedema
can participate in exercise, provided it is
progressed slowly and
their limbs are assessed for any signs of increased or developing
swelling throughout the program and the program is modified accordingly
for each
person.
The key is proper evaluation and assessment for
signs of swelling, tightness, or skin and
tissue changes, before,
during and after exercise.
A related study that we conducted can be found
here involving Upper Extremity
Lymphedema Secondary to Breast
Cancer. The study involved patients with unilateral
upper extremity
lymphedema secondary to axillary node dissection (accompanying
lumpectomy or mastectomy for carcinoma of the breast). It was done to
evaluate the
persistence of reduction in lymphedema following a
single course of Complex
Lymphedema Therapy.
Please write us
any questions or concerns you may have about treatment options at
Lymphedema Therapy.
Our Certified Lymphedema Specialists will be
happy to answer your questions on how
we may help you or someone
you know who has lymphedema. We invite you to fill out
and submit
your questions to us here on our Contact Form.
The physicians and certified
lymphedema therapists at Lymphedema Therapy are
experienced in these
assessments. For more information, contact our center at 516-364-
2200
References:
1.Nieman, David C. Exercise Testing and
Prescription: A Health Related Approach, 4th
ed. Mountain View,
California, Mayfield Publishing Co., 1999: P, 190-205.
2.Casley-Smith,
Judith R, Casley Smith, John R. Modern Treatment for Lymphoedema,
5th ed. Adelaide, Australia, The Lymphology Association of Australia,
1997: p. 188-189.
3.Harris, Susan R, Niesen-Vertommen, Sherri. Challenging
the Myth of Exercise-
Induced Lymphedema Following Breast Cancer: A
Series of Case Reports. Journal of
Surgical Oncology 2000;
74:94-99.
--------------------------------------------------------------------------------
Lymphedema
Therapy
77 Froehlich Farm Blvd., Woodbury, New York 11797
1-800-MD-LYMPH
or (516) 364-2200
Marvin Boris, MD
Stanley Weindorf, MD
Bonnie B.
Lasinski, MA, PT, CI, CLT-LANA
-------
Lymphland
International Lymphedema Online
"Illustration
Courtesy of the American
Cancer Society"
Message
from Yahoo Babel Fish:
Please upgrade to the Microsoft Translator
widget.
What's
this?
Page updated 8/6/09
Email Tina