Use of Stem Cells in Lymphedema
Post Mastectomy (SCL)
This study has
been completed.
First Received on April 20, 2010. Last Updated on March 23,
2011 History
of Changes
Sponsor:
Hospital Universitario Dr. Jose E.
Gonzalez
Information
provided by:
Hospital Universitario Dr. Jose E.
Gonzalez
ClinicalTrials.gov
Identifier:
NCT01112189
Purpose
The post-mastectomy lymphedema
is a complication of removal of the breast and nodal plexus that causes
accumulation of lymph and subsequent enlargement of the upper limb. It is the
most common complication of all attributable to mastectomy with axillary
dissection and which occurs in one third of patients who undergo radical
mastectomy and radiotherapy post-operation. Currently the treatment of
lymphedema of the upper limb is mainly the use of compression stockings, the use
of pneumatic compression pumps and physiotherapy.
Multiple reports indicate that
endothelial progenitor cells (EPC) can differentiate into various cell lines,
reproduced and participate in neoangiogenesis. This study was conducted in the
General Surgery Service, of the Hospital Universitario "Dr. José Eleuterio
González "and proposes the EPC obtained autologous transplantation of bone
marrow for the treatment of postoperative lymphedema in upper limb following
axillary lymphadenectomy through the stimulation of lymphatic neoangiogenesis.
The investigators studied 20 female patients over 18 years after axillary
lymphadenectomy. The objective is to develop an innovative and definitive
treatment for these patients and to analyze the costs and complications that
this treatment may have.
Condition
Intervention
Phase
Lymphedema
Breast
Cancer
Procedure: Autologous transplant
Other: Compressed sleeve treatment
Phase 1
Phase
2
Study Type:
Interventional
Study Design:
Allocation: Non-Randomized
Endpoint
Classification: Safety/Efficacy Study
Intervention Model: Parallel
Assignment
Masking: Open Label
Primary Purpose: Treatment
Official Title:
Postoperative Lymphedema
Treatment in Upper Extremities Following Axillary Lymphadenectomy by
Transplanting Autologous Endothelial Progenitor Cells
(EPC)
Resource links provided by NLM:
Genetics Home Reference related topics:
breast cancer
MedlinePlus related topics: Breast CancerCancerLymphedemaMastectomyU.S.
FDA Resources
Further study details as provided by Hospital Universitario
Dr. Jose E. Gonzalez:
Primary Outcome Measures:
Secondary Outcome Measures:
Enrollment:
20
Study Start Date:
September 2009
Study Completion Date:
September 2010
Primary Completion Date:
August 2010 (Final data collection date for
primary outcome measure)
Arms
Assigned Interventions
Experimental: Patients with stem cells
Patients that receive the stem
cells treatment
Procedure: Autologous transplant
Patients will be stimulated 3
days with Filgrastrim 300 micrograms per day. On the 4th day the autologous
transplant of stem cells will be performed.
Other Name: Stem Cells
transplant
Active Comparator: Compressed sleeve treatment
Patients that will receive the
compressed sleeve treatment
Other: Compressed sleeve treatment
Week 1-2: With compressed sleeve
treatment.
Week 3 -4: Without
treatment.
Week 5 - 6: With compressed
sleeve treatment
Other Name: Compressive sleeve
treatment
Detailed Description:
Phase 1:
The procedure will be as
follows:
10 patients were recruited in
the General Surgery or Oncology meeting the inclusion criteria. During the
study, patients can´t use any other kind of treatment for the lymphedema.
Visit 1: We explain the
procedure by inviting patients to participate after signing informed consent.
There will be a complete medical history, review of inclusion and exclusion
criteria, signing a letter of informed consent, be requested general laboratory
tests (blood count, biochemical profile), tele-ray.
Visit 2: Initiation colony
stimulating factor (Filgrastim SC) to 300 micrograms per day for 3 consecutive
days.
Visit 3: Conduct a puncture and
bone marrow harvesting under local anesthesia of the posterior iliac crest with
Jamshidi needle to aspirate (approximately 50 - 100ml). The product obtained
will be centrifuged in a refrigerated centrifuge at 3500 Sigma EK15 ® rpm/15
minutes to 8 ° C with HES 6% (pentastarch 6g/100ml) to obtain the mononuclear
cell layer. Once the cells were obtained will be transported to the operating
room to manage the patient by intramuscular injection of 0.5 to 1 ml in 30 to 50
sites of the affected limb with a depth of about one centimeter, using a needle
number 25. The administration will take place in the operating room under local
anesthesia or sedation if necessary.
Visit 4 and subsequent: clinical
evaluation will be conducted each week, especially data monitoring of infection
in the puncture sites. At week 12 post-cell infusion, the latest revision will
be made and carried out measurements in both arms to conclude and determine the
outcome of treatment.
Phase 2 (Control group):
Another 10 patients with
lymphedema will be included in a 6 week study to compare the most common
treatment of the lymphedema, the compressed sleeves.
Visit 1: A complete medical
history will be performed. A compression sleeve will be given to the patients
for their use during the next 2 weeks.
Visit 2 and 3: On week 2 and 3
of the compression sleeve treatment, the patients will be measured in both upper
extremities as well as assess the symptoms or not that patients present.
Visit 4 and 5: Patients will
stop using the compression sleeve treatment for the next 2 weeks measured both
upper extremities and interrogate patients about symptoms during this
period.
Visit 6 and 7: The last 2 weeks
of the study patients will be asked to restart the compressed sleeves treatment
and measured both upper extremities and interrogate patients about symptoms
presented during this stage of the study.
Eligibility
Ages Eligible for Study:
18 Years to 75 Years
Genders Eligible for Study:
Female
Accepts Healthy Volunteers:
No
Criteria
Inclusion criteria:
Exclusion criteria:
Contacts and Locations
Please refer to this study by
its ClinicalTrials.gov identifier: NCT01112189
Locations
Mexico
Hospital Universitario Dr Jose
Eleuterio Gonzalez
Monterrey, Nuevo León,
Mexico, 64810
Sponsors and Collaborators
Hospital Universitario Dr. Jose E.
Gonzalez
Investigators
Principal Investigator:
Gerardo E. Muñoz Maldonado,
MD
Hospital Universitario Dr Jose
Eleuterio Gonzalez
More Information
Additional Information:
General Surgery Hospital Universitario Dr. Jose Eleuterio
González
Publications:
Thomas-MacLean R, Miedema B, Tatemichi SR. Breast cancer-related
lymphedema: women's experiences with an underestimated condition. Can Fam
Physician. 2005 Feb;51:246-7.
Levine M; Steering Committee on Clinical Practice Guidelines for
the Care and Treatment of Breast Cancer. Clinical practice guidelines for the
care and treatment of breast cancer: adjuvant systemic therapy for node-positive
breast cancer (summary of the 2001 update). The Steering Committee on Clinical
Practice Guidelines for the Care and Treatment of Breast Cancer. CMAJ. 2001 Mar
6;164(5):644-6. No abstract available.
Bumpers HL, Best IM, Norman D, Weaver WL. Debilitating
lymphedema of the upper extremity after treatment of breast cancer. Am J Clin
Oncol. 2002 Aug;25(4):365-7.
Kim H, Dumont DJ. Molecular mechanisms in lymphangiogenesis:
model systems and implications in human disease. Clin Genet. 2003
Oct;64(4):282-92. Review.
Additional
publications automatically indexed to this study by ClinicalTrials.gov
Identifier (NCT Number):
Maldonado GE, Pérez CA, Covarrubias EE, Cabriales SA, Leyva LA,
Pérez JC, Almaguer DG. Autologous stem cells for the treatment of
post-mastectomy lymphedema: a pilot study. Cytotherapy. 2011
Nov;13(10):1249-55.
Responsible Party:
Dr. med Gerardo Enrique Muñoz Maldonado, Hospital
Universitario "Dr. José Eleuterio González"
ClinicalTrials.gov Identifier:
NCT01112189History
of Changes
Other Study ID Numbers:
CG08-005
Study First Received:
April 20, 2010
Last Updated:
March 23, 2011
Health Authority:
Mexico: Ethics
Committee
A path to treatment of
lymphedema
October 13, 2010
Lymphedema, or swelling
because of the impaired flow of lymph fluid, can occur as a consequence of
cancer or cancer treatment. Chemotherapy can damage lymph ducts, and often
surgeons remove lymph nodes that may be affected by cancer metastasis.
Lymphedema can result in painful swelling, impaired mobility and changes in
appearance.
Emory scientists, led by cardiologist and stem cell biologist Young-sup
Yoon, have shown that they can isolate progenitor cells for the
lining of lymph ducts. This finding could lead to doctors being able to
regenerate and repair lymph ducts using a patient’s own cells. The results are
described in a paper published recently in the journal
Circulation.
The authors used the cell surface marker podoplanin as a handle for isolating
the progenitor cells from bone marrow. Previous research has demonstrated that
podoplanin is essential for the development of the
lymphatic system.
In the paper, the authors use several animal
models to show that the progenitor cells could contribute to the formation of
new lymph ducts, both by becoming part of the lymph ducts and by stimulating the
growth of nearby cells.
“This lymphatic vessel–forming capability can be used for the treatment of
lymphedema or chronic unhealed wounds,” Yoon says.
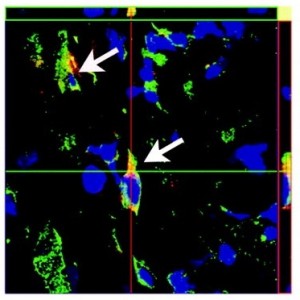
Isolated lymphatic endothelial cells (red)
incorporate into lymph ducts (green) in a model of wound healing in
mice.
The authors also show that mice with tumors show an increase in the number of
this type of circulating progenitor cells. This suggests that tumors send out
signals that encourage lymph duct growth – a parallel to the well-known ability of
tumors to drive growth of blood vessels nearby. Yoon says the presence of these
cells could be a marker for tumor growth and metastasis. Because tumors often
metastasize along lymph ducts and into lymph nodes, studying this type of cells
could lead to new targets for blocking tumor metastasis.
A recent review in the journal Genes
& Development summarizes additional functions of the
lymphatic system in fat metabolism, obesity, inflammation, and the regulation of
salt storage in hypertension.
Post Mastectomy (SCL)
This study has
been completed.
First Received on April 20, 2010. Last Updated on March 23,
2011 History
of Changes
Sponsor:
Hospital Universitario Dr. Jose E.
Gonzalez
Information
provided by:
Hospital Universitario Dr. Jose E.
Gonzalez
ClinicalTrials.gov
Identifier:
NCT01112189
Purpose
The post-mastectomy lymphedema
is a complication of removal of the breast and nodal plexus that causes
accumulation of lymph and subsequent enlargement of the upper limb. It is the
most common complication of all attributable to mastectomy with axillary
dissection and which occurs in one third of patients who undergo radical
mastectomy and radiotherapy post-operation. Currently the treatment of
lymphedema of the upper limb is mainly the use of compression stockings, the use
of pneumatic compression pumps and physiotherapy.
Multiple reports indicate that
endothelial progenitor cells (EPC) can differentiate into various cell lines,
reproduced and participate in neoangiogenesis. This study was conducted in the
General Surgery Service, of the Hospital Universitario "Dr. José Eleuterio
González "and proposes the EPC obtained autologous transplantation of bone
marrow for the treatment of postoperative lymphedema in upper limb following
axillary lymphadenectomy through the stimulation of lymphatic neoangiogenesis.
The investigators studied 20 female patients over 18 years after axillary
lymphadenectomy. The objective is to develop an innovative and definitive
treatment for these patients and to analyze the costs and complications that
this treatment may have.
Condition
Intervention
Phase
Lymphedema
Breast
Cancer
Procedure: Autologous transplant
Other: Compressed sleeve treatment
Phase 1
Phase
2
Study Type:
Interventional
Study Design:
Allocation: Non-Randomized
Endpoint
Classification: Safety/Efficacy Study
Intervention Model: Parallel
Assignment
Masking: Open Label
Primary Purpose: Treatment
Official Title:
Postoperative Lymphedema
Treatment in Upper Extremities Following Axillary Lymphadenectomy by
Transplanting Autologous Endothelial Progenitor Cells
(EPC)
Resource links provided by NLM:
Genetics Home Reference related topics:
breast cancer
MedlinePlus related topics: Breast CancerCancerLymphedemaMastectomyU.S.
FDA Resources
Further study details as provided by Hospital Universitario
Dr. Jose E. Gonzalez:
Primary Outcome Measures:
- Determine if the stem cells are effective in
patients with lymphedema with the decreased of the volume of the affected limb
and improvement of the symptomatology. [ Time Frame: 3 months ] [ Designated as
safety issue: Yes ]
Patients will be measured in 4
different areas of both arms with a tape measure, before the transplant and
weekly after the transplant for 3 months.
Measure 1: 10 cm over the
epicondyle. Measure 2: 5 cm over the the epicondyle. Measure 3: 5 cm under the
the epicondyle. Measure 4: 15 cm under the the epicondyle Also a questionnaire
of the most common symptoms will be given to the patients to mark their own
symptoms before the transplant and 3 months after the
transplant.
Secondary Outcome Measures:
- Participants with Adverse Events as a Measure of
Safety and Tolerability. [ Time Frame: 3 months ] [ Designated as safety issue:
Yes ]
Enrollment:
20
Study Start Date:
September 2009
Study Completion Date:
September 2010
Primary Completion Date:
August 2010 (Final data collection date for
primary outcome measure)
Arms
Assigned Interventions
Experimental: Patients with stem cells
Patients that receive the stem
cells treatment
Procedure: Autologous transplant
Patients will be stimulated 3
days with Filgrastrim 300 micrograms per day. On the 4th day the autologous
transplant of stem cells will be performed.
Other Name: Stem Cells
transplant
Active Comparator: Compressed sleeve treatment
Patients that will receive the
compressed sleeve treatment
Other: Compressed sleeve treatment
Week 1-2: With compressed sleeve
treatment.
Week 3 -4: Without
treatment.
Week 5 - 6: With compressed
sleeve treatment
Other Name: Compressive sleeve
treatment
Detailed Description:
Phase 1:
The procedure will be as
follows:
10 patients were recruited in
the General Surgery or Oncology meeting the inclusion criteria. During the
study, patients can´t use any other kind of treatment for the lymphedema.
Visit 1: We explain the
procedure by inviting patients to participate after signing informed consent.
There will be a complete medical history, review of inclusion and exclusion
criteria, signing a letter of informed consent, be requested general laboratory
tests (blood count, biochemical profile), tele-ray.
Visit 2: Initiation colony
stimulating factor (Filgrastim SC) to 300 micrograms per day for 3 consecutive
days.
Visit 3: Conduct a puncture and
bone marrow harvesting under local anesthesia of the posterior iliac crest with
Jamshidi needle to aspirate (approximately 50 - 100ml). The product obtained
will be centrifuged in a refrigerated centrifuge at 3500 Sigma EK15 ® rpm/15
minutes to 8 ° C with HES 6% (pentastarch 6g/100ml) to obtain the mononuclear
cell layer. Once the cells were obtained will be transported to the operating
room to manage the patient by intramuscular injection of 0.5 to 1 ml in 30 to 50
sites of the affected limb with a depth of about one centimeter, using a needle
number 25. The administration will take place in the operating room under local
anesthesia or sedation if necessary.
Visit 4 and subsequent: clinical
evaluation will be conducted each week, especially data monitoring of infection
in the puncture sites. At week 12 post-cell infusion, the latest revision will
be made and carried out measurements in both arms to conclude and determine the
outcome of treatment.
Phase 2 (Control group):
Another 10 patients with
lymphedema will be included in a 6 week study to compare the most common
treatment of the lymphedema, the compressed sleeves.
Visit 1: A complete medical
history will be performed. A compression sleeve will be given to the patients
for their use during the next 2 weeks.
Visit 2 and 3: On week 2 and 3
of the compression sleeve treatment, the patients will be measured in both upper
extremities as well as assess the symptoms or not that patients present.
Visit 4 and 5: Patients will
stop using the compression sleeve treatment for the next 2 weeks measured both
upper extremities and interrogate patients about symptoms during this
period.
Visit 6 and 7: The last 2 weeks
of the study patients will be asked to restart the compressed sleeves treatment
and measured both upper extremities and interrogate patients about symptoms
presented during this stage of the study.
Eligibility
Ages Eligible for Study:
18 Years to 75 Years
Genders Eligible for Study:
Female
Accepts Healthy Volunteers:
No
Criteria
Inclusion criteria:
- Patients with postsurgical lymphedema in upper
extremities following axillary lymphadenectomy. - Female gender.
- Age over 18 years.
- Patients who wish to participate in the
study. - Informed consent signed.
Exclusion criteria:
- Patients with hypercoagulable states.
- Patients with a history of obstructive vascular
disease in the brain, kidneys or heart. - Patients with congestive heart failure (ejection
fraction less than 30%) - Active infectious process, serious, anywhere in
the body. - Patients over 75 years of
age.
Contacts and Locations
Please refer to this study by
its ClinicalTrials.gov identifier: NCT01112189
Locations
Mexico
Hospital Universitario Dr Jose
Eleuterio Gonzalez
Monterrey, Nuevo León,
Mexico, 64810
Sponsors and Collaborators
Hospital Universitario Dr. Jose E.
Gonzalez
Investigators
Principal Investigator:
Gerardo E. Muñoz Maldonado,
MD
Hospital Universitario Dr Jose
Eleuterio Gonzalez
More Information
Additional Information:
General Surgery Hospital Universitario Dr. Jose Eleuterio
González
Publications:
Thomas-MacLean R, Miedema B, Tatemichi SR. Breast cancer-related
lymphedema: women's experiences with an underestimated condition. Can Fam
Physician. 2005 Feb;51:246-7.
Levine M; Steering Committee on Clinical Practice Guidelines for
the Care and Treatment of Breast Cancer. Clinical practice guidelines for the
care and treatment of breast cancer: adjuvant systemic therapy for node-positive
breast cancer (summary of the 2001 update). The Steering Committee on Clinical
Practice Guidelines for the Care and Treatment of Breast Cancer. CMAJ. 2001 Mar
6;164(5):644-6. No abstract available.
Bumpers HL, Best IM, Norman D, Weaver WL. Debilitating
lymphedema of the upper extremity after treatment of breast cancer. Am J Clin
Oncol. 2002 Aug;25(4):365-7.
Kim H, Dumont DJ. Molecular mechanisms in lymphangiogenesis:
model systems and implications in human disease. Clin Genet. 2003
Oct;64(4):282-92. Review.
Additional
publications automatically indexed to this study by ClinicalTrials.gov
Identifier (NCT Number):
Maldonado GE, Pérez CA, Covarrubias EE, Cabriales SA, Leyva LA,
Pérez JC, Almaguer DG. Autologous stem cells for the treatment of
post-mastectomy lymphedema: a pilot study. Cytotherapy. 2011
Nov;13(10):1249-55.
Responsible Party:
Dr. med Gerardo Enrique Muñoz Maldonado, Hospital
Universitario "Dr. José Eleuterio González"
ClinicalTrials.gov Identifier:
NCT01112189History
of Changes
Other Study ID Numbers:
CG08-005
Study First Received:
April 20, 2010
Last Updated:
March 23, 2011
Health Authority:
Mexico: Ethics
Committee
A path to treatment of
lymphedema
October 13, 2010
Lymphedema, or swelling
because of the impaired flow of lymph fluid, can occur as a consequence of
cancer or cancer treatment. Chemotherapy can damage lymph ducts, and often
surgeons remove lymph nodes that may be affected by cancer metastasis.
Lymphedema can result in painful swelling, impaired mobility and changes in
appearance.
Emory scientists, led by cardiologist and stem cell biologist Young-sup
Yoon, have shown that they can isolate progenitor cells for the
lining of lymph ducts. This finding could lead to doctors being able to
regenerate and repair lymph ducts using a patient’s own cells. The results are
described in a paper published recently in the journal
Circulation.
The authors used the cell surface marker podoplanin as a handle for isolating
the progenitor cells from bone marrow. Previous research has demonstrated that
podoplanin is essential for the development of the
lymphatic system.
In the paper, the authors use several animal
models to show that the progenitor cells could contribute to the formation of
new lymph ducts, both by becoming part of the lymph ducts and by stimulating the
growth of nearby cells.
“This lymphatic vessel–forming capability can be used for the treatment of
lymphedema or chronic unhealed wounds,” Yoon says.
Isolated lymphatic endothelial cells (red)
incorporate into lymph ducts (green) in a model of wound healing in
mice.
The authors also show that mice with tumors show an increase in the number of
this type of circulating progenitor cells. This suggests that tumors send out
signals that encourage lymph duct growth – a parallel to the well-known ability of
tumors to drive growth of blood vessels nearby. Yoon says the presence of these
cells could be a marker for tumor growth and metastasis. Because tumors often
metastasize along lymph ducts and into lymph nodes, studying this type of cells
could lead to new targets for blocking tumor metastasis.
A recent review in the journal Genes
& Development summarizes additional functions of the
lymphatic system in fat metabolism, obesity, inflammation, and the regulation of
salt storage in hypertension.
Cell therapy for the
treatment of lower limb lymphedema. Case report
Terapia celular en el tratamiento de
linfedema de miembros inferiores. Presentación de un caso
Dr. Pedro Goicoechea-DíazI; Prof.
DrC. Porfirio Hernández-RamírezII; Dr. Heriberto
Artaza-SanzI; Dr. Lázaro Cortina-RosalesII; Dra. Vianed
Marsán-SuárezII; Dr. Yamilé Peña-QuíanIII; Dr. Alejandro
Perera-PintadoIII
I Hospital General Docente "Enrique
Cabrera". Ciudad de La Habana, Cuba.
II Instituto de Hematología e Inmunología. Ciudad de
La Habana, Cuba.
III Centro
de Investigaciones Clínicas. Ciudad de La Habana, Cuba.
ABSTRACT
Although lymphedema is a common disabling
disease causing significant morbidity for affected patients, treatment for this
condition remains limited and largely ineffective. Some reported data suggest
that some bone-marrow derived cells may play a role in lymphangiogenesis. It
appears that blood vessels and lymphatic vessels might use the same population
of cells for vasculogenesis and lymphangiogenesis. Therefore, adult stem cell
therapy could be a new useful strategy for the treatment of lymphedema. We
report a resolution of a severe lower limb bilateral lymphedema after
implantation of autologous adult stem cells derived from bone marrow. As far as
we know, this is the first reported case with chronic lower limb lymphedema
treated successfully with autologous cell therapy. This procedure is a
low-cost, relatively simple and easy to perform option that opens new ways for
the treatment of lymphedema.
Key words: Stem cell, lymphedema,
bone-marrow derived cells, lymphangiogenesis.
RESUMEN
Aunque el linfedema es una enfermedad crónica inhabilitante común
que causa morbilidad significativa en los pacientes afectados, el tratamiento
para esta enfermedad se mantiene muy limitada y en la mayor parte de los casos
resulta ineficaz. Algunos datos reportados sugieren que algunas de las células
madre derivadas de la medula ósea pueden intervenir en la linfangiogénesis. Al
parecer, los vasos sanguíneos y los vasos linfáticos podrían usar la misma
población celular para la vasculogénesis y la linfangiogénesis. Por
consiguiente, la terapia con células madre adultas podría ser una nueva
estrategia útil para el tratamiento de linfedema. En el presente trabajo se
informa la resolución de un linfedema bilateral severo de miembros inferiores
después de la implantación de células madre autólogas derivadas de la médula
ósea. Hasta donde sabemos, este es el primer caso de linfedema crónico de los
miembros inferiores tratado exitosamente con células madre autólogas. Este
método de tratamiento es económico, relativamente simple, fácil de realizar y
una opción que abre nuevas vías para el tratamiento del linfedema.
Palabras clave: células madre,
linfedema, células derivadas de la médula ósea, linfangiogénesis.
INTRODUCTION
Lymphedema is a chronic condition characterized
by the abnormal accumulation of interstitial fluid due to insufficiency of the
lymphatic system, either as a primary or as a secondary disorder. Although it
is a common disabling disease causing significant morbidity for affected
patients, treatment for this condition remains limited and largely
ineffective.1
Recently stem-cell based therapy has been the
focus of attention for inducing therapeutic angiogenesis and the therapeutic
potential of adult stem cells in the treatment of peripheral arterial disease
has become increasingly evident during the last years.2
Some reported data suggest that some
bone-marrow derived cells may play a role in lymphangiogenesis.3,4
It appears that blood vessels and lymphatic vessels might use the same
population of cells for vasculogenesis and lymphangiogenesis.5
Therefore, adult stem cell therapy could be a new useful strategy for the
treatment of lymphedema.
Here we report a resolution of a severe lower
limb bilateral lymphedema after implantation of autologous adult stem cells
derived from bone marrow.
CASE REPORT
A 58 -year -old man was referred to our service
of angiology with severe swelling of both lower extremities. This swelling
started two years earlier after recurrent episodes of lymphangitis. The
diagnosis of lymphedema of the inflammatory type was performed and conservative
therapy was initiated, including compression bandaging. Despite this treatment
the swelling became progressively more severe. This condition limited his
walking in a marked degree and disabled him to go upstairs.
Except the above mentioned lymphangitis
episodes, the patient did not have a noteworthy past medical history. Physical
examination revealed a body weight of 137 kg, a blood pressure of 120/80 mm Hg
and severe lower limb bilateral lymphedema affecting both extremities up to the
inguinal regions (fig. 1A). No other pathological findings were
revealed. The circumferences of his lower extremities were measured 7 cm above
the knee, at the knee, 7cm below the knee, at the ankles and at the metatarsus
(table).
Laboratory findings, including a complete blood
count, sedimentation rate, urinalysis findings, liver function tests and renal
tests were unremarkable. A chest radiograph and an electrocardiogram showed
normal results. A 99mTc sulphide colloidal
lymphoscintigraphy6 showed absence of flow at both lower
extremities.
As patient was considered unresponsive to
conservative therapy, taking into account worsening of swelling in both
extremities as well as serious worsening in quality of life, an autologous
transplantation of Granulocyte Colony-Stimulating Factor (G-CSF) mobilized
peripheral blood stem cell (PBSC) in the most affected extremity was proposed.
Scientific and Ethics Committees of participating institutions approved this
treatment and the patient gave written informed consent.
For bone marrow mononuclear cell mobilization,
the patient was previously subcutaneously injected with human recombinant G-CSF
(Leuko CIM, CIMAB SA, La Habana, Cuba). The whole procedure, including
peripheral blood collection and mononuclear cell (MNC) concentration adding
hidroxyetilstarch (HES) 6 % to the collected blood, was performed as previously
described.7 A final volume of 140 mL of concentrated cell suspension
was obtained. Absolute MNC count was 8,4 x 109 and CD34+ absolute
stem cell number was 42 x 106. Cell viability was 95 %.
Under propofol 1 %, sedation and in sterile
conditions concentrated cells were implanted in the most affected extremity
(right limb) by multiple circumferential injections into the leg and distal
half of the thigh. In addition, cells were also injected into the dorsum of the
foot. A volume of 0,75 mL of the cell suspension was implanted 1-1,5 cm deep
into each injection site with a 3 x 3 cm grid, using a 24 - gauge needle. Total
injection volume was 120 mL.
Slight leakage of fluid from the tissues
observed at the injection sites, disappeared 48 hours after cell implantation.
During this period, compression bandaging was used and there after an elastic
stocking was indicated. No other related side- effect was observed throughout
the therapeutic procedure or within the whole follow-up period.
One week after cell implantation a mild
improvement of foot swelling was appreciated at the treated extremity.
Subsequently, progressive improvement of lymphedema was observed and striking
improvement of bilateral lymphedema was obtained with 19 kg body weight lost
during the 6 months following cell implantation (fig. 1B). Six months after
treatment the patient showed reduced circumferences of both extremities
(table). Follow-up lymphoscintigraphy was not performed because patient did not
accept this study. Improvement was sustained during one and a half year
follow-up.
DISCUSSION
In recent years, much attention has been given
to lymphangiogenesis and new advances in the study of lymphedema have been
obtained.8
Lymphatic vessels and blood vessels are
essential collaborating parts of the circulatory system. The lymphatic vessels
differ in many ways from the blood vessels, but they also share many
properties. Recently, new information about the regulation of lymphangiogenesis
has been gained, and the factors known to regulate blood vessels have been
shown to be involved in the biology of the lymphatic vessels.9 The
development of blood and lymphatic vascular systems is primarily regulated by
vascular endothelial growth factor (VEGF) family members: VEGF-A, VEGF-B,
VEGF-C, VEGF-D and placenta growth factor.10 It is considered that
VEGF-A is the most important of them for the control of angiogenesis, whereas
VEGF-C and VEGF-D are the main factors that control lymphangiogenesis.
From the clinical point, various therapeutic
procedures have been proposed for selected patients with lymphedema, who are
unresponsive to conservative therapy.8,9 Several surgical options
with promising results have been reported, including lymphatic microsurgery,
autologous lymphatic tissue implants and circumferential suction - assisted
lipectomy.8,11-13
More recently, based on novel findings on the
molecular mechanisms involved in lymphangiogenesis, encouraging results have
been obtained with VEGF-C gene therapy and with human recombinant VEGF-C in
experimental animal models, which provide attractive procedures for
pro-lymphoangiogenic therapy in lymphedema.14,15 Known similarities
between the regulation of blood and lymphatic vessels, and the preclinical and
clinical studies that have provided evidence that implantation of bone marrow
derived cells into ischemic limbs can improve tissue vascularization,
encouraged us to use cell therapy for the treatment of lymphedema.
Following autologous mobilized PBSC
implantation, our case showed an astonishing clinical recovery with marked
improvement of bilateral lymphedema, despite the fact that cells were implanted
in only one of the affected extremities.
Up today, the mechanisms through which the
transplanted cells might improve tissue recovery remain unknown. Several
hypothesis have been suggested including transdifferentiation, cell fusion, a
paracrine effect by release of various cytokines and growth factors or maybe an
addition of more than one mechanism.5,16,17 It has been referred
that adult human progenitor cells from bone marrow are potent sources of
VEGF.17,18 On this point, it is important to underline that VEGF-C
and VEGF-D are specific regulators of lymphangiogenesis.10
It is accepted that hematopoietic cells may
release different growth factors and cytokines and a fraction of CD34+ cells
may acts as lymphatic / vascular endothelial precursors cells.2,3
There are at least two possibilities that might
explain why G-CSF mobilization plus the transplantation into local affected
tissues of the collected and concentrated PBSCs can result in the excellent
therapeutic improvement obtained. The first is that local injections of G-CSF
mobilized PBSCs into the selected lower extremity directly bring a number of
circulating endothelial precursor cells into affected tissues where these cells
can initiate lymphangiogenesis. The second is that a large number of
transplanted cells can secrete in vivo in the injected sites several
cytokines and grown factors known to stimulate lymphangiogenesis and that may
produce a paracrine effect in a similar way as has been suggested in ischemic
diseases.17,19 Another possible related mechanism is based on the
in vivo (endogenous) availability of a pool of systemic and circulating
G-CSF mobilized PBSCs that might be recruited to the affected tissues,
contributing in this way to lymphangiogenesis. Some of these possibilities may
coexist in this therapeutic approach.
By the other side, we were surprised by the
fact that the contralateral, also affected but non-treated, lower limb, also
showed a notable improvement. Although we have not a proved explanation for the
mechanisms involved in this therapy related effect, it could be suggested that
endogenous mobilized PBSCs were recruited to the affected tissues in this limb,
as aforementioned, and in this way they could in principle act similarly to the
local exogenous transplanted cells facilitating the recovery of the swollen
tissues inducing certain degree of lymphangiogenesis. As a pure speculation,
this observation raises also the possibility that the classical inter cellular
coordinative communicating system may be more complex thanpreviously thought.
In some cases increased serum values of
cytokines and growth factors secreted by the exogenously implanted cells have
been detected.20 Perhaps, a telecrine effect of these circulating
soluble products might exist in certain cases with an action on distant
target-cells; this effect might be in addition to the paracrine effect
previously suggested. This possibility would help to explain in part our result
and also others not yet completely explained, related to improvement of glucose
metabolism in diabetic patients who received mononuclear cell implantation into
the lower extremities because of ischemic disorders.21,22
As far as we know, this is the first reported
case with chronic lower limb lymphedema treated successfully with autologous
cell therapy. This method of treatment is a low-cost, relatively simple and
easy to perform option that opens new ways for the treatment of lymphedema. Our
observation is supported by the results obtained in a recent controlled study
in patients with breast cancer related arm lymphedema.23
However, further studies are needed in order to
obtain an accurate evaluation of the efficacy and long term safety of this
novel therapeutic strategy in patients with lymphedema.
REFERENCES
1. Yoon YS, Marayama T, Gravereux E, Tkebuchava
T, Silver M, Curry C, et al. VEGF-C gene therapy augments postnatal
lymphangiogenesis and ameliorates secondary lymphedema. J Clin Invest
2003;111:717-25.
2. Hernández P, Cortina L, Artaza H, Pol N, Lam
RM, Dorticós E, et al. Autologous bone-marrow mononuclear cell implantation in
patients with severe lower limb ischaemia: A comparison of using blood cell
separator and Ficoll density gradient centrifugation. Atherosclerosis
2007;194:e52-6.
3. Rafii S, Lyden D. Therapeutic stem and
progenitor cell transplantation for organ vascularization and regeneration. Nat
Med 2003;9:702-12.
4. Salven P, Mustjoki S, Alitalo R, Alitalo K,
Raffi S. VEGFR-3 and CD 133 identify a population of CD 34+ lymphatic/vascular
endothelial precursor cells. Blood 2003;101:168-72.
5. Religa P, Cao R, Biorndahl M, Zhou Z, Zhu Z,
Cao Y, et al. Presence of bone marrow-derived circulating progenitor
endothelial cells in the newly formed lymphatic vessels. Blood
2005;106:4184-90.
6. Lee AF. Lymphoscintigraphy of the
extremities. In: O´Connor MK, editor. The Mayo Clinical Manual of Nuclear
Medicine. New York: Churchill Livingstone; 1996. pp. 513-9.
7. Hernández P, Artaza H, Díaz AJ, Cortina LD,
Lam RM, Pol N, et al. Autotrasplante de células madre adultas en miembros
inferiores con isquemia crítica. Experiencia en Cuba. Rev Esp Invest Quirúrg
2007;10:204-11.
8. Warren AG, Brorson H, Borud LJ, Slavin SA.
Lymphedema: A comprehensive review. Ann Plast Surg 2007;59:464-72.
9. Jussila L, Alitalo K. Vascular growth
factors and lymphangiogenesis. Physiol Rev 2002;8:673-700.
10. Sato Y. VEGFR1 for lymphangiogenesis
arterioscler. Tromb Vasc Biol 2008;28:604-5.
11. Campisi D, Davini D, Bellini C, Taddei G,
Villa G, Fulcheri E, et al. Lymphatic microsurgery for the treatment of
lymphedema. Microsurgery 2006;26:65-9.
12. Campisi C, Da Rin E, Bellini C, Bonioli E,
Boccardo F. Pediatric lymphedema and correlated syndromes: Rle of microsurgery.
Microsurgery 2008;28:138-42.
13. Belcaro G, Errichi BM, Cesarone MR,
Ippolito E, Dugall M, Ledda A, et al. Lymphatic tissue transplant in lymphedema
a minimally invasive, out patient, surgical method: a 10-year follow-up pilot
study. Angiology 2008;59:77-83.
14. Cao R, Eriksson A, Kubo H, Alitalo K, Cao
Y, Thyberg J. Comparative evaluation of FGF-2, VEGF-A, and VEGF-C induced
angiogenesis, lymphangiogenesis, vascular fenestrations, and permeability. Circ
Res 2004;95:664-70.
15. Lohela M, Saaristo A, Veikkola T, Alitalo
K. Lymphangiogenic growth factors, receptors and therapies. Thromb Haemost
2003;90:167-84.
16. Körbling M, de Lima MJ, Thomas E, Khanna A,
Najjar AM, Gu J, et al. Fusion of circulating blood cells with solid organ
tissue cells in clinical stem cell transplant: A potential therapeutic model?
Reg Med 2008;3:157-64.
17. Méndez-Otero R, de Freitas GR, Andre C,
Furtado de Mendoça ML, Friedrich M, Oliveira-Filho J. Potential roles of bone
marrow stem cells in stroke therapy. Regen Med 2007;2:417-23.
18. Wang M, Crisotomo PR, Herring C, Meldrum
KK, Meldrum DR. Human progenitor cells from bone marrow or adipose tissue
produce VEGF, HGF, and IGF-I in response to TNF by a p38 MAPK-dependent
mechanism. Am J Physiol Regul Integr Comp Physiol 2006;291:880-4.
19. De Araujo JD, de Araujo Filho JD, Ciorlin
E, Ruiz MA, Ruiz LP, Greco OT, et al. A terapia celular no tratamento da
isquemia crítica dos miembros inferiores. J Vas Bras 2005;4:357-65.
20. Tachi Y, Fukui D, Wada Y, Koshikawa M,
Shimodaira S, Ikeda U, et al. Changes in angiogenesis related factors in serum
following autologous bone marrow cell implantation for severe limb ischemia.
Exp Opin Biol Ther 2008;8:705-12.
21. Huang P, Li S, Han M, Xiao Z, Yang R, Han
ZC. Autologous transplantation of granulocyte colony-stimulating factor -
mobilized peripheral blood mononuclear cells improves critical limb ischemia in
diabetes. Diabetes Care 2005;28:2155-60.
22. Novoa E, Medina A. Therapeutic angiogenesis
in arterial ischaemic limbs by autologous bone marrow transplantation (ABMT).
The Conzi´s effect in human diabetes mellitus. Arch Med Int (Uruguay)
2007;29(Suppl 1):S24-S25.
23. Hou C, Wu X, Jin X. Autologous bone marrow
stromal cells transplantation for the treatment of secondary arm lymphedema: A
prospective controlled study in patients with breast cancer related lymphedema.
Jpn J Clin Oncol 2008;38:670-4.
Recibido: 8 de junio del 2010.
Aprobado: 25 de junio dle 2010.
Prof. DrC. Porfirio Hernández Ramírez.
Instituto de Hematología e Inmunología. Apartado 8070, CP 10800, Ciudad de La
Habana, Cuba. Tel (537) 643 8695, 8268. Fax (537) 644 2334. E-mail: [email protected]
Cytotherapy. 2011
Nov;13(10):1249-55. doi: 10.3109/14653249.2011.594791.
Autologous stem cells for the treatment of post-mastectomy lymphedema: a
pilot study.
Maldonado GE, Pérez CA, Covarrubias EE, Cabriales SA, Leyva LA, Pérez JC, Almaguer DG.
Source
Hospital Universitario 'Dr José Eleuterio González', Universidad Autónoma de
Nuevo León, México. [email protected]
Abstract
BACKGROUND AIMS. Lymphedema is a common complication with breast cancer
treatment that does not have a definite cure. Our objective was to determine the
efficacy of autologous stem cells (ASC) in the treatment of lymphedema secondary
to mastectomy and axillary lymphadenectomy in comparison with traditional
decongestive treatment with compression sleeves. METHODS. A prospective study
including 20 women with lymphedema secondary to breast cancer surgery with
axillary lymphadenectomy was conducted. Women were assigned at random to one of
two groups. One group of 10 women was injected with ASC in the affected arm,
whereas the other 10 women comprised the control group and received traditional
compression sleeve therapy (CST). The follow-up for both groups was 12 weeks.
Pain, sensitivity and mobility were assessed before and after therapy. RESULTS.
There was improvement in the volume of lymphedema in both groups, with no
significant difference. In the ASC group there was an overall volume reduction
during the follow-up, whereas in the CST group lymphedema recurred after the
compression sleeve was removed. CONCLUSIONS. Our findings suggest that ASC
injection for patients with lymphedema can be an effective treatment. It reduces
arm volume and associated co-morbidities of pain and decreased sensitivity.
Traditional CST was also effective for lymphedema reduction, but it was
dependent on continuous use of the treatment.
PMID:
21999374
[PubMed - indexed for MEDLINE]
treatment of lower limb lymphedema. Case report
Terapia celular en el tratamiento de
linfedema de miembros inferiores. Presentación de un caso
Dr. Pedro Goicoechea-DíazI; Prof.
DrC. Porfirio Hernández-RamírezII; Dr. Heriberto
Artaza-SanzI; Dr. Lázaro Cortina-RosalesII; Dra. Vianed
Marsán-SuárezII; Dr. Yamilé Peña-QuíanIII; Dr. Alejandro
Perera-PintadoIII
I Hospital General Docente "Enrique
Cabrera". Ciudad de La Habana, Cuba.
II Instituto de Hematología e Inmunología. Ciudad de
La Habana, Cuba.
III Centro
de Investigaciones Clínicas. Ciudad de La Habana, Cuba.
ABSTRACT
Although lymphedema is a common disabling
disease causing significant morbidity for affected patients, treatment for this
condition remains limited and largely ineffective. Some reported data suggest
that some bone-marrow derived cells may play a role in lymphangiogenesis. It
appears that blood vessels and lymphatic vessels might use the same population
of cells for vasculogenesis and lymphangiogenesis. Therefore, adult stem cell
therapy could be a new useful strategy for the treatment of lymphedema. We
report a resolution of a severe lower limb bilateral lymphedema after
implantation of autologous adult stem cells derived from bone marrow. As far as
we know, this is the first reported case with chronic lower limb lymphedema
treated successfully with autologous cell therapy. This procedure is a
low-cost, relatively simple and easy to perform option that opens new ways for
the treatment of lymphedema.
Key words: Stem cell, lymphedema,
bone-marrow derived cells, lymphangiogenesis.
RESUMEN
Aunque el linfedema es una enfermedad crónica inhabilitante común
que causa morbilidad significativa en los pacientes afectados, el tratamiento
para esta enfermedad se mantiene muy limitada y en la mayor parte de los casos
resulta ineficaz. Algunos datos reportados sugieren que algunas de las células
madre derivadas de la medula ósea pueden intervenir en la linfangiogénesis. Al
parecer, los vasos sanguíneos y los vasos linfáticos podrían usar la misma
población celular para la vasculogénesis y la linfangiogénesis. Por
consiguiente, la terapia con células madre adultas podría ser una nueva
estrategia útil para el tratamiento de linfedema. En el presente trabajo se
informa la resolución de un linfedema bilateral severo de miembros inferiores
después de la implantación de células madre autólogas derivadas de la médula
ósea. Hasta donde sabemos, este es el primer caso de linfedema crónico de los
miembros inferiores tratado exitosamente con células madre autólogas. Este
método de tratamiento es económico, relativamente simple, fácil de realizar y
una opción que abre nuevas vías para el tratamiento del linfedema.
Palabras clave: células madre,
linfedema, células derivadas de la médula ósea, linfangiogénesis.
INTRODUCTION
Lymphedema is a chronic condition characterized
by the abnormal accumulation of interstitial fluid due to insufficiency of the
lymphatic system, either as a primary or as a secondary disorder. Although it
is a common disabling disease causing significant morbidity for affected
patients, treatment for this condition remains limited and largely
ineffective.1
Recently stem-cell based therapy has been the
focus of attention for inducing therapeutic angiogenesis and the therapeutic
potential of adult stem cells in the treatment of peripheral arterial disease
has become increasingly evident during the last years.2
Some reported data suggest that some
bone-marrow derived cells may play a role in lymphangiogenesis.3,4
It appears that blood vessels and lymphatic vessels might use the same
population of cells for vasculogenesis and lymphangiogenesis.5
Therefore, adult stem cell therapy could be a new useful strategy for the
treatment of lymphedema.
Here we report a resolution of a severe lower
limb bilateral lymphedema after implantation of autologous adult stem cells
derived from bone marrow.
CASE REPORT
A 58 -year -old man was referred to our service
of angiology with severe swelling of both lower extremities. This swelling
started two years earlier after recurrent episodes of lymphangitis. The
diagnosis of lymphedema of the inflammatory type was performed and conservative
therapy was initiated, including compression bandaging. Despite this treatment
the swelling became progressively more severe. This condition limited his
walking in a marked degree and disabled him to go upstairs.
Except the above mentioned lymphangitis
episodes, the patient did not have a noteworthy past medical history. Physical
examination revealed a body weight of 137 kg, a blood pressure of 120/80 mm Hg
and severe lower limb bilateral lymphedema affecting both extremities up to the
inguinal regions (fig. 1A). No other pathological findings were
revealed. The circumferences of his lower extremities were measured 7 cm above
the knee, at the knee, 7cm below the knee, at the ankles and at the metatarsus
(table).
Laboratory findings, including a complete blood
count, sedimentation rate, urinalysis findings, liver function tests and renal
tests were unremarkable. A chest radiograph and an electrocardiogram showed
normal results. A 99mTc sulphide colloidal
lymphoscintigraphy6 showed absence of flow at both lower
extremities.
As patient was considered unresponsive to
conservative therapy, taking into account worsening of swelling in both
extremities as well as serious worsening in quality of life, an autologous
transplantation of Granulocyte Colony-Stimulating Factor (G-CSF) mobilized
peripheral blood stem cell (PBSC) in the most affected extremity was proposed.
Scientific and Ethics Committees of participating institutions approved this
treatment and the patient gave written informed consent.
For bone marrow mononuclear cell mobilization,
the patient was previously subcutaneously injected with human recombinant G-CSF
(Leuko CIM, CIMAB SA, La Habana, Cuba). The whole procedure, including
peripheral blood collection and mononuclear cell (MNC) concentration adding
hidroxyetilstarch (HES) 6 % to the collected blood, was performed as previously
described.7 A final volume of 140 mL of concentrated cell suspension
was obtained. Absolute MNC count was 8,4 x 109 and CD34+ absolute
stem cell number was 42 x 106. Cell viability was 95 %.
Under propofol 1 %, sedation and in sterile
conditions concentrated cells were implanted in the most affected extremity
(right limb) by multiple circumferential injections into the leg and distal
half of the thigh. In addition, cells were also injected into the dorsum of the
foot. A volume of 0,75 mL of the cell suspension was implanted 1-1,5 cm deep
into each injection site with a 3 x 3 cm grid, using a 24 - gauge needle. Total
injection volume was 120 mL.
Slight leakage of fluid from the tissues
observed at the injection sites, disappeared 48 hours after cell implantation.
During this period, compression bandaging was used and there after an elastic
stocking was indicated. No other related side- effect was observed throughout
the therapeutic procedure or within the whole follow-up period.
One week after cell implantation a mild
improvement of foot swelling was appreciated at the treated extremity.
Subsequently, progressive improvement of lymphedema was observed and striking
improvement of bilateral lymphedema was obtained with 19 kg body weight lost
during the 6 months following cell implantation (fig. 1B). Six months after
treatment the patient showed reduced circumferences of both extremities
(table). Follow-up lymphoscintigraphy was not performed because patient did not
accept this study. Improvement was sustained during one and a half year
follow-up.
DISCUSSION
In recent years, much attention has been given
to lymphangiogenesis and new advances in the study of lymphedema have been
obtained.8
Lymphatic vessels and blood vessels are
essential collaborating parts of the circulatory system. The lymphatic vessels
differ in many ways from the blood vessels, but they also share many
properties. Recently, new information about the regulation of lymphangiogenesis
has been gained, and the factors known to regulate blood vessels have been
shown to be involved in the biology of the lymphatic vessels.9 The
development of blood and lymphatic vascular systems is primarily regulated by
vascular endothelial growth factor (VEGF) family members: VEGF-A, VEGF-B,
VEGF-C, VEGF-D and placenta growth factor.10 It is considered that
VEGF-A is the most important of them for the control of angiogenesis, whereas
VEGF-C and VEGF-D are the main factors that control lymphangiogenesis.
From the clinical point, various therapeutic
procedures have been proposed for selected patients with lymphedema, who are
unresponsive to conservative therapy.8,9 Several surgical options
with promising results have been reported, including lymphatic microsurgery,
autologous lymphatic tissue implants and circumferential suction - assisted
lipectomy.8,11-13
More recently, based on novel findings on the
molecular mechanisms involved in lymphangiogenesis, encouraging results have
been obtained with VEGF-C gene therapy and with human recombinant VEGF-C in
experimental animal models, which provide attractive procedures for
pro-lymphoangiogenic therapy in lymphedema.14,15 Known similarities
between the regulation of blood and lymphatic vessels, and the preclinical and
clinical studies that have provided evidence that implantation of bone marrow
derived cells into ischemic limbs can improve tissue vascularization,
encouraged us to use cell therapy for the treatment of lymphedema.
Following autologous mobilized PBSC
implantation, our case showed an astonishing clinical recovery with marked
improvement of bilateral lymphedema, despite the fact that cells were implanted
in only one of the affected extremities.
Up today, the mechanisms through which the
transplanted cells might improve tissue recovery remain unknown. Several
hypothesis have been suggested including transdifferentiation, cell fusion, a
paracrine effect by release of various cytokines and growth factors or maybe an
addition of more than one mechanism.5,16,17 It has been referred
that adult human progenitor cells from bone marrow are potent sources of
VEGF.17,18 On this point, it is important to underline that VEGF-C
and VEGF-D are specific regulators of lymphangiogenesis.10
It is accepted that hematopoietic cells may
release different growth factors and cytokines and a fraction of CD34+ cells
may acts as lymphatic / vascular endothelial precursors cells.2,3
There are at least two possibilities that might
explain why G-CSF mobilization plus the transplantation into local affected
tissues of the collected and concentrated PBSCs can result in the excellent
therapeutic improvement obtained. The first is that local injections of G-CSF
mobilized PBSCs into the selected lower extremity directly bring a number of
circulating endothelial precursor cells into affected tissues where these cells
can initiate lymphangiogenesis. The second is that a large number of
transplanted cells can secrete in vivo in the injected sites several
cytokines and grown factors known to stimulate lymphangiogenesis and that may
produce a paracrine effect in a similar way as has been suggested in ischemic
diseases.17,19 Another possible related mechanism is based on the
in vivo (endogenous) availability of a pool of systemic and circulating
G-CSF mobilized PBSCs that might be recruited to the affected tissues,
contributing in this way to lymphangiogenesis. Some of these possibilities may
coexist in this therapeutic approach.
By the other side, we were surprised by the
fact that the contralateral, also affected but non-treated, lower limb, also
showed a notable improvement. Although we have not a proved explanation for the
mechanisms involved in this therapy related effect, it could be suggested that
endogenous mobilized PBSCs were recruited to the affected tissues in this limb,
as aforementioned, and in this way they could in principle act similarly to the
local exogenous transplanted cells facilitating the recovery of the swollen
tissues inducing certain degree of lymphangiogenesis. As a pure speculation,
this observation raises also the possibility that the classical inter cellular
coordinative communicating system may be more complex thanpreviously thought.
In some cases increased serum values of
cytokines and growth factors secreted by the exogenously implanted cells have
been detected.20 Perhaps, a telecrine effect of these circulating
soluble products might exist in certain cases with an action on distant
target-cells; this effect might be in addition to the paracrine effect
previously suggested. This possibility would help to explain in part our result
and also others not yet completely explained, related to improvement of glucose
metabolism in diabetic patients who received mononuclear cell implantation into
the lower extremities because of ischemic disorders.21,22
As far as we know, this is the first reported
case with chronic lower limb lymphedema treated successfully with autologous
cell therapy. This method of treatment is a low-cost, relatively simple and
easy to perform option that opens new ways for the treatment of lymphedema. Our
observation is supported by the results obtained in a recent controlled study
in patients with breast cancer related arm lymphedema.23
However, further studies are needed in order to
obtain an accurate evaluation of the efficacy and long term safety of this
novel therapeutic strategy in patients with lymphedema.
REFERENCES
1. Yoon YS, Marayama T, Gravereux E, Tkebuchava
T, Silver M, Curry C, et al. VEGF-C gene therapy augments postnatal
lymphangiogenesis and ameliorates secondary lymphedema. J Clin Invest
2003;111:717-25.
2. Hernández P, Cortina L, Artaza H, Pol N, Lam
RM, Dorticós E, et al. Autologous bone-marrow mononuclear cell implantation in
patients with severe lower limb ischaemia: A comparison of using blood cell
separator and Ficoll density gradient centrifugation. Atherosclerosis
2007;194:e52-6.
3. Rafii S, Lyden D. Therapeutic stem and
progenitor cell transplantation for organ vascularization and regeneration. Nat
Med 2003;9:702-12.
4. Salven P, Mustjoki S, Alitalo R, Alitalo K,
Raffi S. VEGFR-3 and CD 133 identify a population of CD 34+ lymphatic/vascular
endothelial precursor cells. Blood 2003;101:168-72.
5. Religa P, Cao R, Biorndahl M, Zhou Z, Zhu Z,
Cao Y, et al. Presence of bone marrow-derived circulating progenitor
endothelial cells in the newly formed lymphatic vessels. Blood
2005;106:4184-90.
6. Lee AF. Lymphoscintigraphy of the
extremities. In: O´Connor MK, editor. The Mayo Clinical Manual of Nuclear
Medicine. New York: Churchill Livingstone; 1996. pp. 513-9.
7. Hernández P, Artaza H, Díaz AJ, Cortina LD,
Lam RM, Pol N, et al. Autotrasplante de células madre adultas en miembros
inferiores con isquemia crítica. Experiencia en Cuba. Rev Esp Invest Quirúrg
2007;10:204-11.
8. Warren AG, Brorson H, Borud LJ, Slavin SA.
Lymphedema: A comprehensive review. Ann Plast Surg 2007;59:464-72.
9. Jussila L, Alitalo K. Vascular growth
factors and lymphangiogenesis. Physiol Rev 2002;8:673-700.
10. Sato Y. VEGFR1 for lymphangiogenesis
arterioscler. Tromb Vasc Biol 2008;28:604-5.
11. Campisi D, Davini D, Bellini C, Taddei G,
Villa G, Fulcheri E, et al. Lymphatic microsurgery for the treatment of
lymphedema. Microsurgery 2006;26:65-9.
12. Campisi C, Da Rin E, Bellini C, Bonioli E,
Boccardo F. Pediatric lymphedema and correlated syndromes: Rle of microsurgery.
Microsurgery 2008;28:138-42.
13. Belcaro G, Errichi BM, Cesarone MR,
Ippolito E, Dugall M, Ledda A, et al. Lymphatic tissue transplant in lymphedema
a minimally invasive, out patient, surgical method: a 10-year follow-up pilot
study. Angiology 2008;59:77-83.
14. Cao R, Eriksson A, Kubo H, Alitalo K, Cao
Y, Thyberg J. Comparative evaluation of FGF-2, VEGF-A, and VEGF-C induced
angiogenesis, lymphangiogenesis, vascular fenestrations, and permeability. Circ
Res 2004;95:664-70.
15. Lohela M, Saaristo A, Veikkola T, Alitalo
K. Lymphangiogenic growth factors, receptors and therapies. Thromb Haemost
2003;90:167-84.
16. Körbling M, de Lima MJ, Thomas E, Khanna A,
Najjar AM, Gu J, et al. Fusion of circulating blood cells with solid organ
tissue cells in clinical stem cell transplant: A potential therapeutic model?
Reg Med 2008;3:157-64.
17. Méndez-Otero R, de Freitas GR, Andre C,
Furtado de Mendoça ML, Friedrich M, Oliveira-Filho J. Potential roles of bone
marrow stem cells in stroke therapy. Regen Med 2007;2:417-23.
18. Wang M, Crisotomo PR, Herring C, Meldrum
KK, Meldrum DR. Human progenitor cells from bone marrow or adipose tissue
produce VEGF, HGF, and IGF-I in response to TNF by a p38 MAPK-dependent
mechanism. Am J Physiol Regul Integr Comp Physiol 2006;291:880-4.
19. De Araujo JD, de Araujo Filho JD, Ciorlin
E, Ruiz MA, Ruiz LP, Greco OT, et al. A terapia celular no tratamento da
isquemia crítica dos miembros inferiores. J Vas Bras 2005;4:357-65.
20. Tachi Y, Fukui D, Wada Y, Koshikawa M,
Shimodaira S, Ikeda U, et al. Changes in angiogenesis related factors in serum
following autologous bone marrow cell implantation for severe limb ischemia.
Exp Opin Biol Ther 2008;8:705-12.
21. Huang P, Li S, Han M, Xiao Z, Yang R, Han
ZC. Autologous transplantation of granulocyte colony-stimulating factor -
mobilized peripheral blood mononuclear cells improves critical limb ischemia in
diabetes. Diabetes Care 2005;28:2155-60.
22. Novoa E, Medina A. Therapeutic angiogenesis
in arterial ischaemic limbs by autologous bone marrow transplantation (ABMT).
The Conzi´s effect in human diabetes mellitus. Arch Med Int (Uruguay)
2007;29(Suppl 1):S24-S25.
23. Hou C, Wu X, Jin X. Autologous bone marrow
stromal cells transplantation for the treatment of secondary arm lymphedema: A
prospective controlled study in patients with breast cancer related lymphedema.
Jpn J Clin Oncol 2008;38:670-4.
Recibido: 8 de junio del 2010.
Aprobado: 25 de junio dle 2010.
Prof. DrC. Porfirio Hernández Ramírez.
Instituto de Hematología e Inmunología. Apartado 8070, CP 10800, Ciudad de La
Habana, Cuba. Tel (537) 643 8695, 8268. Fax (537) 644 2334. E-mail: [email protected]
Cytotherapy. 2011
Nov;13(10):1249-55. doi: 10.3109/14653249.2011.594791.
Autologous stem cells for the treatment of post-mastectomy lymphedema: a
pilot study.
Maldonado GE, Pérez CA, Covarrubias EE, Cabriales SA, Leyva LA, Pérez JC, Almaguer DG.
Source
Hospital Universitario 'Dr José Eleuterio González', Universidad Autónoma de
Nuevo León, México. [email protected]
Abstract
BACKGROUND AIMS. Lymphedema is a common complication with breast cancer
treatment that does not have a definite cure. Our objective was to determine the
efficacy of autologous stem cells (ASC) in the treatment of lymphedema secondary
to mastectomy and axillary lymphadenectomy in comparison with traditional
decongestive treatment with compression sleeves. METHODS. A prospective study
including 20 women with lymphedema secondary to breast cancer surgery with
axillary lymphadenectomy was conducted. Women were assigned at random to one of
two groups. One group of 10 women was injected with ASC in the affected arm,
whereas the other 10 women comprised the control group and received traditional
compression sleeve therapy (CST). The follow-up for both groups was 12 weeks.
Pain, sensitivity and mobility were assessed before and after therapy. RESULTS.
There was improvement in the volume of lymphedema in both groups, with no
significant difference. In the ASC group there was an overall volume reduction
during the follow-up, whereas in the CST group lymphedema recurred after the
compression sleeve was removed. CONCLUSIONS. Our findings suggest that ASC
injection for patients with lymphedema can be an effective treatment. It reduces
arm volume and associated co-morbidities of pain and decreased sensitivity.
Traditional CST was also effective for lymphedema reduction, but it was
dependent on continuous use of the treatment.
PMID:
21999374
[PubMed - indexed for MEDLINE]
| therapeutic_lymphang_using_stem_vegf_c_hydrogel.pdf | |
| File Size: | 2041 kb |
| File Type: | |